A Deep Dive into Lung Anatomy and Functionality

Article Overview
Purpose of the Article
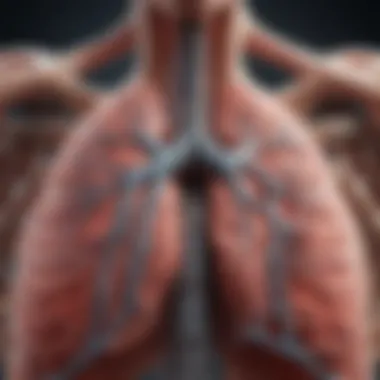
This article aims to provide a detailed exploration of lung anatomy, offering insights into its structure and the critical functions it performs in the human body. It addresses the lung's external features and internal organization while also considering the vascular systems that support respiratory processes. The goal is to enhance understanding for both science enthusiasts and industry professionals, making the complex nature of the lungs accessible to a wider audience.
Relevance to Multiple Disciplines
Understanding lung anatomy is not solely the domain of medical professionals; rather, its relevance stretches across various fields, including biology, environmental science, and education. For students, it provides foundational knowledge essential for advanced studies. Researchers can utilize this information to explore connections between anatomy and various respiratory conditions. Educators can develop richer curricula that reflect real-world application.
Research Background
Historical Context
The study of lung anatomy has evolved significantly, tracing back centuries. Ancient texts, such as those from Hippocrates, laid the groundwork by noting the lungs' connection to both health and disease. In more recent history, William Harvey’s discoveries in the 17th century about circulation contributed to understanding how blood flow impacts lung function. This historical progression underscores the significance of lungs beyond mere breathing; they play a vital role in the body's overall physiology.
Key Concepts and Definitions
To explore the anatomy of the lungs comprehensively, it is essential to clarify some key concepts:
- Bronchi: The main passageways into the lungs, branching off from the trachea.
- Alveoli: Tiny air sacs where gas exchange occurs; their structure is crucial for efficient oxygen absorption.
- Pleura: The double-layered membrane surrounding each lung, facilitating smooth movement during respiration.
- Lobes: The lungs are divided into lobes; the right lung has three, while the left has two, accommodating better heart placement.
The lungs are not just organs of respiration but also play essential roles in metabolism, the immune response, and even fluid regulation within the body.
The lungs are not just organs of respiration but also play essential roles in metabolism, the immune response, and even fluid regulation within the body.
In this article, we will delve deeper into these components, reviewing their anatomy, functionality, and significance in health and disease. With the latest research findings and insights shared throughout, readers can expect an enriching experience that underscores the lungs' remarkable complexity.
Foreword to Lung Anatomy
Understanding lung anatomy is more than just a biological endeavor; it's a journey into one of the most vital systems in our body. The lungs do not merely facilitate breathing; they play a crucial role in oxygenating blood, maintaining pH balance, and filtering dust and pathogens. Grasping the structure and function of the lungs allows us to appreciate their significance in both health and disease.
The exploration of lung anatomy encompasses various elements. First, it emphasizes the intricate architectural design of the lungs, which includes lobes, bronchi, and alveoli, and showcases their unique functionalities. Furthermore, comprehension of this anatomy lays a solid foundation for understanding respiratory physiology. This knowledge can have substantial implications for those studying medicine, nursing, or any health-related field.
When considering lung anatomy, one must also take into account its evolution over time. Historical context enriches our understanding and leads us to appreciate how far medical science has come. It sheds light on groundbreaking discoveries and advances that have led to improvement in diagnostics and treatments for lung-related ailments.
Ultimately, this exploration not only caters to students and professionals but is also essential for anyone interested in the biological sciences, as it fosters a broad comprehension of how our bodies function, adapt, and sometimes succumb to various pathologies.
In essence, the study of lung anatomy encapsulates the intersection of structure, function, and clinical importance, thereby creating a comprehensive guide to this critical organ system.
Overview of Lung Importance
The lungs hold an irreplaceable position in the human body. They not only facilitate the exchange of gases—oxygen entering the bloodstream and carbon dioxide being expelled—but also influence other bodily functions, such as regulating blood pH and influencing even our immune responses.
- Gas Exchange: The lungs are the primary site for oxygen intake and carbon dioxide removal, essential for cellular respiration.
- Acid-Base Balance: By regulating blood CO2 levels, the lungs play a vital role in maintaining pH levels, which is crucial for various physiological processes.
- Defense Mechanisms: The airway epithelium is equipped with cilia and mucus to trap pathogens and particles, safeguarding the body from infections.
- Voice Production: The lungs support speech by providing the necessary airflow. This function is crucial in communication and social interaction.
Given their multifaceted roles, learning about the lungs reveals much about overall health, potential diseases, and effective treatments.
Historical Perspectives
The understanding of lung anatomy has evolved through centuries, shaped by notable historical figures and significant discoveries.
- Ancient Understanding: Early medical practitioners like Hippocrates acknowledged the lungs’ importance, albeit with rudimentary knowledge. They believed air had vital qualities that contributed to life.
- Vesalius’s Contributions: Andreas Vesalius, during the Renaissance, shifted paradigms by insisting on the importance of direct observation in anatomy, leading to more accurate descriptions of lung structure.
- Modern Insights: In the 20th century, advancements like imaging techniques and fiber-optic bronchoscopy transformed our understanding, enabling detailed explorations of lung structures.
Today, our comprehension of lung anatomy is underpinned by invaluable contributions from scientists and researchers, paving the way for advancements in fields such as pulmonology and thoracic surgery.
"The lungs are not just organs of respiration, but gateways to understanding health, disease, and human physiology."
"The lungs are not just organs of respiration, but gateways to understanding health, disease, and human physiology."
In a nutshell, a historical lens on lung anatomy provides insight into the progression of medical knowledge, illustrating how continuous inquiry and discovery have shaped our contemporary understanding.
Structural Foundations
Understanding the anatomy of the lungs requires a solid grasp of their structural foundations. This section delves into the core elements driving lung function, emphasizing how the physical layout of the lungs impacts respiratory processes. The organization of lung structures not only aids in efficient gas exchange but also ensures protection from environmental stressors. A thorough exploration of these foundational aspects provides insight into both health and disease states, enhancing our appreciation of lung complexity.
Lobes and Lobules
The lungs consist of distinct lobes and lobules that play crucial roles in their functionality. By dissecting these components, we can better understand how each segment contributes to overall respiratory health.
Characteristics of Lobes
The lungs are divided into lobes, with the right lung boasting three lobes and the left only two, allowing it to accommodate the heart. This arrangement is a fundamental characteristic of lung anatomy, and its significance can't be overstated. Each lobe works independently yet in harmony, giving us a robust mechanism for breathing. The lobes contain bronchi, bronchioles, and alveoli, forming the basic units where gas exchange happens.
A key characteristic of these lobes is their capacity for expansion. The expansive nature allows for intricate manipulation of air volume during inhalation and exhalation. This adaptability is often found to be beneficial for enhancing oxygen intake under various conditions, especially during physical exertion.
One unique feature is the presence of connective tissue partitions between the lobes, which helps limit the spread of infection should one lobe be compromised. However, there can be disadvantages as well; if an infection does spread, it may tax the entire lung system, leading to more severe respiratory issues.
Function of Lobules
Diving deeper, lobules represent the functional subdivisions within each lobe. Lobules work as autonomous units that contain clusters of alveoli. The distinction between lobes and lobules is essential for comprehending lung functionality and pathology.
The primary characteristic of lobules is their specialization. Each lobule is designed to optimize gas exchange efficiency, featuring its own network of capillaries. This set-up makes it possible for the lungs to respond swiftly to varying oxygen demands of the body. This specialized functioning allows for efficient management of oxygen and carbon dioxide, making it a popular feature in discussions about lung anatomy.
A notable point is the proximity of the lobules to blood vessels, which facilitates rapid gas diffusion. However, this can also be disadvantageous if lobules become inflamed; localized swelling can impair overall function, jeopardizing adequate respiratory performance.
Bronchial Tree Architecture
The architecture of the bronchial tree is another critical area in lung anatomy that deserves attention. This network not only channels air to the lungs but also plays a role in protecting lung tissue from pathogens and particles.
Trachea and Main Bronchi
The trachea serves as the primary airway, splitting into the left and right main bronchi. This branching is a fundamental aspect of airway design, allowing efficient airflow to both lungs. It is crucial for directing inhaled air into the targeted lung areas.
A standout characteristic of the trachea and main bronchi is their structure reinforced by cartilage rings, which prevent collapse during breathing cycles. This architectural feature is particularly beneficial since it ensures a stable airway even when pressures fluctuate dramatically during inhalation and exhalation.
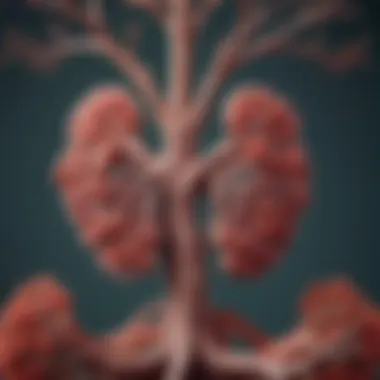

Yet, one must consider the unique feature of the flexible nature of these bronchi. In conditions such as asthma, constriction in these areas can severely hamper airflow, demonstrating both their strengths in normal physiology and vulnerabilities during disease.
Secondary and Tertiary Branching
As members of the bronchial tree, secondary and tertiary bronchi further distribute air throughout the lung. Secondary bronchi branch from the main bronchi and guide air into the lobes while tertiary bronchi continue the branching deep into the lobules.
The key characteristic of these bronchi is their increasing branching complexity. Each division allows the lungs to maximize surface area and contact with alveoli, optimizing gas exchange. This complexity is beneficial in ensuring that every nook and cranny of the lung is well-ventilated and prepared for functional activity.
However, this branching also presents a challenge; narrow passages can become easily obstructed, for instance, during respiratory infections or allergic reactions, leading to compromised airflow. An understanding of this architecture is vital for grasping respiratory pathologies and their interventions.
Airway Epithelium
The airway epithelium stands as a crucial component within the respiratory system, playing a significant role in protecting the lungs from environmental hazards while facilitating gas exchange. This specialized epithelial layer is comprised of various cell types that each contribute uniquely to its fundamental responsibilities. Its functionality is not only key to maintaining respiratory health but also sheds light on the mechanisms underlying several lung diseases.
Cellular Composition
Ciliated Cells
Ciliated cells are one of the primary types of epithelial cells in the respiratory tract. Their most notable characteristic is the presence of tiny hair-like structures called cilia that protrude from the cell surface. These cilia play an essential role in clearing mucus and contaminants from the airways. Acting like an assembly line, they beat in a coordinated rhythm to push mucus upward towards the throat, thus helping to keep the airways clear of debris and pathogens. This aspect makes ciliated cells a beneficial nodal point for respiratory function.
One unique feature of ciliated cells is their ability to regenerate. In cases of injury or damage, they can proliferate and repopulate the airway epithelium, although this process can be slow and may be compromised in chronic diseases. However, their effectiveness diminishes with age and exposure to harmful substances such as tobacco smoke, highlighting a disadvantage.
Club Cells
Club cells, formerly known as Clara cells, are critical for maintaining the integrity of the airway epithelium, particularly in the bronchiolar region. One key characteristic of club cells is their ability to secrete a range of substances, including toxicant-neutralizing enzymes and surfactant-like proteins. This function not only assists in protecting the epithelium from damage but also helps maintain surface tension in the airways, enhancing overall lung function. Their presence is a popular choice for discussions regarding airway biology because they form a defensive line against inhaled toxins.
A unique feature of club cells is their role in the regeneration of the epithelium following injury. When the airway epithelium is damaged, club cells can proliferate and differentiate into ciliated cells, thus aiding recovery. Nonetheless, there can be a downside; in persistent inflammatory conditions, these cells can sometimes proliferate abnormally, contributing to airway remodeling seen in diseases such as asthma.
Basal Cells
Basal cells serve as the stem-like cells of the airway epithelium. They are pivotal in the maintenance and repair of the airway surface. The key characteristic of basal cells is their capability to differentiate into other types of epithelial cells, such as ciliated and club cells. This regenerative capacity makes them a crucial point of focus in the context of lung health.
Basal cells' unique feature includes their ability to sense environmental changes and respond to injury appropriately. They play a critical part in restoring epithelial integrity after damage. On the flip side, in chronic lung diseases, their dysfunctional proliferation may lead to dysplastic changes, resulting in impaired airway function.
Functionality in Mucociliary Clearance
Mucociliary clearance is a vital defense mechanism that involves the coordinated action of ciliated cells and mucus production. The mucus traps inhaled particles, pathogens, and irritants, while the cilia rhythmically expel this debris upwards toward the oral cavity. This process not only protects the airways but also maintains overall lung function by ensuring that the pulmonary regions remain free of potential harmful substances.
In summary, each component of the airway epithelium showcases specialized characteristics and functionalities vital to respiratory health. An understanding of these elements offers insights into how dysfunction can lead to respiratory diseases, emphasizing the overall importance of airway epithelium in the anatomy of lungs.
Alveolar Structures
Alveolar structures represent the intricacies of our lungs, serving as vital components in the intricate ballet of gas exchange. These microscopic air sacs, numbering in the millions, play a crucial role in supplying oxygen to the bloodstream while simultaneously facilitating the removal of carbon dioxide. Understanding their architecture is key to grasping not only the lungs’ function but also how various diseases can significantly hinder respiratory efficiency. Their significance extends beyond simple anatomy; it encompasses how these structures can adapt or falter in response to both environmental challenges and systemic conditions.
Composition of Alveoli
Type and Type Alveolar Cells
Type I and Type II alveolar cells form the backbone of the alveolar structure. Type I cells, which cover about 95% of the alveolar surface area, are thin and flat, optimizing the process of gas exchange due to their large surface area. Their high surface permeabilty ensures that oxygen can move swiftly from alveoli to capillaries while carbon dioxide travels back into the alveoli, ready to be exhaled. This characteristic is paramount, as any impairment can lead to suboptimal gas exchange.
On the other hand, Type II alveolar cells are less abundant but incredibly important. They are cuboidal in shape and secrete surfactant, a substance that decreases surface tension in the alveoli. This action not only prevents alveolar collapse during exhalation but also aids in lung expansion during inhalation, ensuring efficient breathing. Their unique feature is the response to lung injury, as they can proliferate to replace damaged type I cells. This adaptability makes them invaluable, particularly in contexts related to lung repair and regeneration. However, an overproduction of surfactant compensating for lung injury can lead to complications such as also contributing to pulmonary edema.
Alveolar Macrophages
Alveolar macrophages serve as the essential guardians of the lungs, residing within the alveoli. Their primary role is to engulf and digest particulate matter, including pathogens and debris, that infiltrates the lungs. This characteristic defines them as a crucial line of defense against pneumonia and other respiratory infections. They continuously patrol the alveolar spaces, alert for any signs of trouble.
What makes them particularly fascinating is their ability to influence immune responses. They not only digest pathogens but can also emit signaling molecules that orchestrate broader immune reactions throughout the body. This property not only underlines their role in innate immunity but also their involvement in inflammatory processes, which could have implications in chronic lung diseases like asthma or COPD.
However, reliance on macrophages can have its downsides. For instance, excessive inflammation triggered by these cells can lead to damage in the alveoli, affecting gas exchange. Additionally, certain diseases can compromise their function, reducing the lung's cleaning capabilities and allowing infections or irritants to accumulate.
Gas Exchange Mechanisms
The gas exchange mechanisms at work within the alveolar structures are complex yet elegant. The direct contact between alveolar air and the blood within capillaries allows for the rapid transfer of oxygen and carbon dioxide. This is achieved primarily through diffusion, where gases move from areas of higher concentration to lower concentration.
Key factors influencing this essential process include:
- Surface Area: The vast surface area of alveoli facilitates efficient gas exchange.
- Concentration Gradient: The difference in gas concentrations on either side of the alveolar wall drives diffusion.
- Thickness of the Membrane: A thinner barrier (the alveolar-capillary membrane) enhances the exchange efficiency.
Efficient gas exchange is essential, as even minor disruptions can lead to significant health issues.
Efficient gas exchange is essential, as even minor disruptions can lead to significant health issues.
Understanding these mechanisms enhances our insight into various respiratory diseases, such as emphysema, where the destruction of alveolar walls reduces surface area, significantly compromising oxygen uptake and carbon dioxide elimination. As we continue to research these structures, the quest to improve lung health becomes ever more crucial.
Vascular Connections
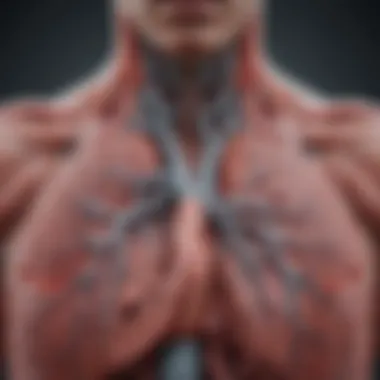
Understanding the vascular connections in the lungs is critical for grasping how oxygen is delivered to the body while ensuring carbon dioxide is expelled. The lungs are more than just air sacs; they are a vital hub of circulatory and respiratory interactions. The synchronicity between the lungs and their blood supply is what enables the efficient functioning of this essential organ.
Pulmonary Circulation
The pulmonary circulation serves a fundamental role in maintaining gas exchange within the lungs. Blood is pumped from the right ventricle of the heart through the pulmonary arteries into the lungs. This process is vital since it directs deoxygenated blood towards the alveoli, where it encounters a high concentration of oxygen.
Once in the lungs, the blood undergoes a transformation. As it flows through the capillaries surrounding the alveoli, oxygen diffuses from the air in the alveoli into the blood, while carbon dioxide moves in the opposite direction to be exhaled. This exchange is essential for sustaining cellular function and preventing respiratory acidosis, a condition that can arise if carbon dioxide accumulates in the bloodstream. The efficiency of pulmonary circulation ensures that the lungs can manage varying demands on oxygen supply, whether during periods of rest or intense physical activity.
Bronchial Circulation
In contrast to pulmonary circulation, bronchial circulation supplies oxygenated blood to the lung tissues themselves. It is provided by the bronchial arteries, which branch off the aorta. This circulation is fundamental for nourishing the lung's structural components, especially the bronchi and bronchioles, ensuring they withstand the mechanical stresses of ventilation.
Furthermore, the bronchial veins carry the deoxygenated blood back to the heart, but they do not contribute to gas exchange like the pulmonary veins do. Instead, they serve a supportive role, maintaining the health of lung tissues and preventing ischemia, which can occur if blood flow is compromised.
This dual vascular system—pulmonary for gas exchange and bronchial for structural integrity—highlights the complexity of lung anatomy.
Each component has its specialized function, yet they operate together seamlessly to ensure our respiratory system remains efficient.
"The lungs, in their elegant architecture, showcase the interplay of structure and function, revealing how critical vascular connections underpin their role in human physiology."
"The lungs, in their elegant architecture, showcase the interplay of structure and function, revealing how critical vascular connections underpin their role in human physiology."

Epilogue
In summary, the vascular connections within the lungs are indispensable for efficient respiration and maintaining pulmonary health. Without the pulmonary and bronchial circulations working in tandem, our bodies wouldn’t receive the necessary oxygen nor be effectively rid of carbon dioxide. Understanding these systems provides valuable insight into how the lungs support life.
Innervation of the Lungs
The innervation of the lungs is a critical component in understanding their function and how they interact with the body as a whole. The lungs do not function in isolation; they are part of a complex system where the nervous system plays a pivotal role. Innervation affects airflow regulation, air quality adjustment, and even responses to irritants or harmful particles. Recognizing how these various components work together can deepen our appreciation for respiratory health and its implications on overall well-being.
Nervous System Input
The lungs receive inputs from both the central and peripheral nervous systems, which modulate their functions effectively. Key players in this orchestration are the vagus nerves, responsible for a significant portion of autonomic control. When you inhale, signals are sent to your lungs through this nerve, stimulating bronchoconstriction when necessary. This ensures that the body maintains proper airflow and gas exchange under varying conditions.
A primary benefit of this intricate innervation is the ability to respond swiftly to changes in physiological demands. For instance, during exercise, the nervous system can increase respiratory rate and tidal volume, ensuring adequate oxygen delivery to meet heightened metabolic needs. Additionally, sensory neurons located in the airways help detect harmful stimuli, relaying information back to the brain to initiate coughing or other protective reflexes. This dual feedback mechanism—detecting and responding—illustrates how essential neural inputs are in lung health.
Role of Autonomic Nervous System
The autonomic nervous system (ANS) divides into two branches: the sympathetic and parasympathetic nervous systems. While the sympathetic system is often associated with the body’s fight-or-flight responses, it actually promotes bronchodilation in the lungs. This response allows for greater airflow when situations demand increased oxygen delivery, such as during physical exertion or stress. On the other hand, the parasympathetic nervous system tends to exert a calming influence, promoting bronchoconstriction and reducing airflow during periods of rest.
The balance between these two forces is paramount. If the sympathetic response is too dominant, it may lead to conditions where chronic bronchodilation occurs, sometimes seen in cases of anxiety or stress. Conversely, overactivity of the parasympathetic branch may contribute to conditions like asthma, where excessive bronchoconstriction hampers breathing.
"Understanding the innervation of the lungs provides critical insights into how we can manipulate these mechanisms for therapeutic gain."
"Understanding the innervation of the lungs provides critical insights into how we can manipulate these mechanisms for therapeutic gain."
In summary, the innervation of the lungs intricately connects the respiratory system with the broader neural framework of the body. By fostering effective communication between these systems, we enhance our ability to adapt to various physical and environmental challenges. The contribution of the autonomic nervous system, in particular, plays a crucial role in modulating respiratory mechanics and overall lung health.
Functional Aspects
Understanding the functional aspects of lung anatomy is critical for grasping how the respiratory system operates. This section sheds light on the intricate processes involved in breathing while considering how various factors contribute to overall respiratory health. It paves the way for appreciating the significance of both mechanical and neurological controls over breathing, thus interlinking structure with function.
Mechanics of Breathing
Breathing is a complex interplay of physical dynamics that enables gas exchange. It's not just about drawing air in and pushing it out; there are mechanics that ensure this process is efficient and effective. Inhalation and exhalation are vital components of this cycle, each characterized by distinct behaviors.
Inhalation Dynamics
Inhalation is an active process primarily driven by the diaphragm and intercostal muscles. When these muscles contract, they create negative pressure within the thoracic cavity, pulling air into the lungs. This transformative action not only enriches the alveolar space with oxygen but also sets the stage for optimal gas exchange. One key characteristic of inhalation dynamics is the importance of lung compliance; it indicates how easily the lungs can expand with the incoming air.
The benefit of understanding inhalation dynamics lies in its capacity to highlight the factors affecting lung capacity and efficiency. For instance, conditions like pulmonary fibrosis can lead to reduced compliance. A unique feature of inhalation is the role of the pleurae, the membranes surrounding the lungs that create a necessary adhesion between the lungs and chest wall. If these were to become inflamed or filled with fluid, inhalation could become compromised. Thus, while inhalation is usually a seamless process, external factors can turn it into a challenge.
Exhalation Dynamics
Exhalation, on the other hand, can be both passive and active, depending on the situation. In a normal resting state, it's primarily passive, driven by the elastic recoil of the lungs and thoracic cavity. However, during vigorous activities, such as exercise, abdominal muscles may assist in forcing air out, making it more forceful. A key characteristic here is that passive exhalation allows for a more efficient respiratory cycle by utilizing the natural elasticity of lung tissues.
One compelling aspect of exhalation dynamics is its role in maintaining optimal carbon dioxide levels in the blood. When utilizing active exhalation during physical exertion, the body can significantly enhance gas exchange by removing CO2 more efficiently, preventing respiratory acidosis. Its unique feature lies in how different conditions, like asthma, can hinder this process, leading to trapped air and breathing difficulties. Understanding these mechanisms provides insight into respiratory health and potential interventions.
Regulation of Breathing
Breathing is not a whimsical act; it's firmly regulated by both chemical and neural inputs, ensuring that our body maintains homeostasis. This regulation becomes particularly important during exercise, sleep, or in response to environmental changes.
Chemical Control
Chemical control of breathing primarily involves detecting changes in carbon dioxide, oxygen, and pH levels within the blood. Chemoreceptors located in the brain, the carotid arteries, and aortic arch sense these fluctuations and send signals to adjust the breathing rate accordingly. The strength of this mechanism lies in its immediacy and responsiveness, ensuring that the body remains in balance.
One appealing aspect of chemical control is its adaptability; it allows the body to cope with varying levels of physical activity or even high-altitude conditions. A notable feature of this control system is the role of bicarbonate buffering to manage pH, safeguarding against acidosis. The downside? Unmanaged conditions like chronic obstructive pulmonary disease can disrupt these mechanisms, leading to ineffective responses. Therefore, understanding chemical control is crucial for recognizing how the body self-regulates.
Neural Control
Neural control of breathing predominantly involves the brainstem structures, particularly the medulla oblongata and pons. This neural network orchestrates the rhythm of breathing by sending signals to the respiratory muscles based on physical needs.
The significance of neural control lies in its ability to integrate and respond quickly to inputs from the body. For example, emotional responses, like stress or excitement, can modify breathing patterns rapidly. Its unique characteristic is the ability to collaborate with other systems, like hormonal responses, to modulate breath intensity and frequency.It is also influenced by higher brain functions, which can override basic patterns when the need arises, such as holding breath while diving.
Conversely, during severe neurological disorders, the communication between the brain and respiratory muscles can be impaired, leading to significant challenges. Grasping how neural control operates gives us insight into certain conditions affecting respiratory health and offers perspectives for treatment.
Developmental Biology
Understanding the developmental biology of the lungs is crucial for several reasons. It not only explicates the complex process by which these organs form but also sheds light on abnormalities during development that can lead to respiratory diseases. From embryonic stages through postnatal adjustments, every phase plays a pivotal role in establishing lung function, morphology, and overall capacity.
Embryonic Development of Lungs
The emergence of lungs begins in the early weeks of embryonic development. This is a carefully choreographed series of events that transform a simple cellular structure into the intricate architecture that supports breathing. It starts with the formation of the respiratory diverticulum, which buds off from the foregut around the fourth week of gestation. This diverticulum eventually gives rise to the trachea, bronchi, and the lung buds.
During this phase, the epithelial cells proliferate and differentiate into various types, setting the stage for future lung functionalities. The mesoderm surrounding the buds provides essential signals that guide the development of the nearby structures, notably blood vessels and airways. As development progresses, interactions between various cell types become critical for normal morphogenesis. Disruptions at this stage can lead to serious conditions like tracheoesophageal fistula or congenital diaphragmatic hernia, underscoring the importance of proper embryonic development.
During prenatal development, the lungs are filled with fluid, and it is only after birth that they expand and fill with air, a transition that is crucial for newborn survival.
During prenatal development, the lungs are filled with fluid, and it is only after birth that they expand and fill with air, a transition that is crucial for newborn survival.
Essentially, the intricate interplay of genetics, environmental signals, and mechanical tension drives the formation of the lungs, making embryonic development an area ripe for exploration in both basic and clinical research.
Postnatal Development Changes
After birth, lungs undergo significant structural and functional changes. Initially, the lungs are not fully developed, and a gradual process of maturation occurs in the first few years of life. Increased lung volume and surface area for gas exchange are the primary changes observed postnatally.
Key aspects include:
- Alveolar Formation: The development of alveoli, where gas exchange occurs, dramatically increases postnatally. From approximately 20 million alveoli at birth, the number expands to over 600 million by the age of eight.
- Elastic Tissue Development: The production of elastic fibers crucial for lung compliance increases, allowing for more efficient expansion and contraction during respiration.
- Capillary Network: The vasculature continues to mature, enhancing blood supply and improving oxygen delivery throughout the developing body.
Surfactant production also becomes increasingly important in this stage, aiding in maintaining alveolar stability and reducing surface tension.
Understanding these processes can provide insights into adult respiratory conditions and potential interventions for those with developmental disruptions. Collectively, the journey from embryonic development to postnatal maturation emphasizes the lungs’ dynamic nature and their adaptability to changing physiological demands.
Pathological Considerations
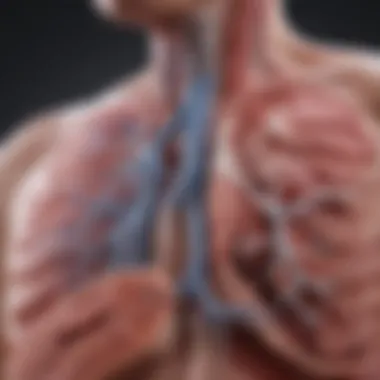
Understanding the anatomical complexities of the lungs goes hand in hand with examining the pathological conditions that afflict them. The pathological considerations section provides vital insights into how various diseases alter lung structure and function. Recognizing the manifestations of disorders like Chronic Obstructive Pulmonary Disease, Asthma, and Lung Cancer not only aids in comprehension of lung anatomy but also underscores the critical interplay between structure and pathology. It’s integral to grasp how environmental factors and habitual behaviors contribute to pulmonary diseases, which invariably influence treatment strategies and outcomes.

Common Lung Diseases
Chronic Obstructive Pulmonary Disease
Chronic Obstructive Pulmonary Disease, commonly known as COPD, represents a major health concern that outlines several critical characteristics that make it a focal point of this article. COPD is primarily marked by two main conditions: chronic bronchitis and emphysema. This duality contributes to airflow limitation and a significant decline in quality of life for those affected. Its relevance in this discourse is underscored by the fact that COPD affects millions and is a leading cause of morbidity and mortality worldwide.
One of the key characteristics of COPD is how it compromises the lung's capacity for gas exchange. This leads to hypoxia, where insufficient oxygen reaches the bloodstream, creating a cascading effect on other bodily functions. The unique feature of COPD worth noting is its progressive nature. Over time, individuals may find themselves increasingly reliant on medical support and therapies, which can involve everything from inhalers to surgical interventions. The disadvantage here is the lifestyle adjustments and financial burden on both individuals and healthcare systems, which are profound.
Asthma
Asthma represents another significant topic within the realm of lung pathology. This condition is characterized by an inflammation of the airways, leading to episodic airflow obstruction. Asthma is particularly noteworthy because it can vary greatly in severity and frequency among individuals; some may experience occasional symptoms, while others encounter frequent debilitating episodes. This sort of variability showcases the dynamic nature of lung diseases.
The key characteristic that stands out in asthma cases is the role of triggers, which can range from allergens to environmental pollutants. These factors can exacerbate the disease and make management complex. The unique feature of asthma is its responsiveness to treatment; many patients can lead normal lives with the aid of inhaled corticosteroids and bronchodilators. However, the potential disadvantage is that severe cases can lead to life-threatening situations, especially if asthma is poorly controlled.
Lung Cancer
Lung Cancer is among the most concerning pathological conditions affecting the lungs. Its connection to anatomical considerations is critical because it showcases how a tumor can alter lung structure and function profoundly. Lung Cancer often arises from the epithelium of the respiratory tract and can manifest in various forms, such as non-small cell lung cancer and small cell lung cancer. This makes it a central topic in discussions about respiratory diseases.
One key characteristic of lung cancer is its often asymptomatic early stages, which can delay diagnosis until it reaches advanced stages. The unique feature of lung cancer lies in its multifaceted treatment approaches, which can include surgery, chemotherapy, and radiation. Each method has its own implications for lung anatomy and function, as treatments can sometimes lead to partial removal of lung tissue or broader systemic effects. The disadvantage of this disease is its overall prognosis; despite advances in medicine, lung cancer remains one of the deadliest cancers, often linked to smoking and environmental toxins, creating a pressing need for preventive measures.
Impact of Environmental Factors
Environmental factors play a significant role in lung health, intertwining with the aforementioned diseases in a multitude of ways. Pollution, smoke inhalation, and occupational hazards are just a few contributors that can sharpen one’s risk profile for developing chronic pulmonary conditions. Understanding these factors underscores the importance of preventative healthcare and policy measures aimed at reducing exposure to harmful substances.
"Environmental influences are foundational in the puzzle of lung health, guiding both disease emergence and progression."
"Environmental influences are foundational in the puzzle of lung health, guiding both disease emergence and progression."
Recognizing how external agents affect lung anatomy and physiology helps contextualize the significance of comprehensive lung health strategies, further bridging the gap between structure and function.
Recent Research Insights
In the ever-evolving field of pulmonary science, recent research insights play a crucial role in enhancing our understanding of lung anatomy and its myriad functions. The exploration of innovative imaging techniques and the emergence of novel therapies not only improve diagnostic accuracy but also pave the way for new treatment paradigms. By staying attuned to these advancements, professionals can better appreciate the complexities facing lung health today.
One of the primary benefits of current research is its ability to shed light on previously elusive aspects of lung structure and function. As researchers delve deeper, they uncover revelations that may shift the paradigms used in clinical and educational settings. This knowledge contributes significantly to improving patient outcomes, guiding interventions and enriching our overall comprehension of pulmonary health.
Innovations in Lung Imaging
Recent advancements in lung imaging technologies have revolutionized the ability to visualize and understand lung anatomy. Techniques such as high-resolution computed tomography (HRCT) and functional magnetic resonance imaging (fMRI) allow for a detailed assessment of lung structures at both macro and micro levels.
- High-Resolution Computed Tomography (HRCT): This technique offers clearer images of lung parenchyma, vital for diagnosing conditions like interstitial lung disease. With its capacity to provide finely detailed images, HRCT allows physicians to visualize small airways and alveoli, offering insights into disease processes that were previously difficult to discern.
- Functional MRI: This method provides dynamic visualizations of lung function. By capturing real-time changes during breathing, fMRI can help evaluate ventilation patterns and regional lung function, which is crucial for conditions such as asthma and chronic obstructive pulmonary disease.
The integration of artificial intelligence (AI) into imaging analysis is another exciting development. Machine learning algorithms are increasingly being employed to assist radiologists in interpreting lung images more efficiently and accurately. This not only reduces the chance of misdiagnosis but also streamlines workflows in busy clinical settings.
"The convergence of AI and lung imaging could redefine diagnostic pathways, enabling earlier detection and improved treatment plans for patients."
"The convergence of AI and lung imaging could redefine diagnostic pathways, enabling earlier detection and improved treatment plans for patients."
Emerging Treatments and Therapies
Alongside improvements in diagnostic techniques, research is also yielding promising treatments that aim to address various lung diseases more effectively. Recent studies have highlighted a number of innovative therapies that are reshaping the approach to pulmonary care.
- Biologics: These therapies are particularly beneficial for asthma and are designed to target specific pathways involved in inflammation. By blocking certain immune responses, they can significantly reduce the frequency of asthma attacks and improve patients’ quality of life.
- Stem Cell Therapy: Emerging research has shown that stem cell therapy may hold promise for repairing damaged lung tissue, particularly in cases of pulmonary fibrosis or severe injury. Although still largely experimental, this innovative approach has the potential to revolutionize treatment by promoting regeneration rather than merely managing symptoms.
- Gene Therapy: There have been strides in gene editing technologies, like CRISPR, which are being explored for treating genetic lung diseases, such as cystic fibrosis. By correcting mutations at the DNA level, gene therapy could offer long-lasting solutions to hereditary conditions that plague patients.
As these new therapies continue to evolve, ongoing clinical trials and research studies are critical for understanding their safety and efficacy. The wealth of knowledge being generated through these investigations ultimately contributes to an enriched perspective on lung health, guiding healthcare professionals in providing cutting-edge care.
Future Perspectives in Lung Research
The field of lung research is on the brink of transformation. With advances in technology and a deeper understanding of lung diseases, the prospects for improving both health outcomes and quality of life are brighter than ever. Research today is not just about addressing existing conditions; it extends to anticipating future challenges and opportunities. This focus opens avenues for more effective treatments and preventive strategies—ultimately benefiting both individuals and healthcare systems alike.
Contemporary Challenges
Despite strides made in lung research, various challenges persist. Understanding the complexity of lung diseases is one of the foremost hurdles. For instance, the intermingling of genetic, environmental, and lifestyle factors complicates the ability to pinpoint specific causes of conditions such as asthma or chronic obstructive pulmonary disease. Furthermore, the COVID-19 pandemic has exposed gaps in our understanding of lung complications resulting from viral infections. As researchers scramble to analyze the implications on lung health, the need for comprehensive, multi-faceted approaches grows stronger.
Another pressing issue is the persistence of health disparities among populations. Factors such as socioeconomic status and access to healthcare can lead to unequal outcomes in lung health. Tackling these disparities requires not only innovative research but also active collaborations between community leaders, healthcare providers, and researchers.
Potential Areas for Exploration
Advancements in Regenerative Medicine
Regenerative medicine stands at the frontier of lung research, offering groundbreaking possibilities. This field leverages the body's own regenerative capabilities to repair or replace damaged tissues. One major aspect of regenerative medicine is the utilization of stem cell therapy, which has shown promise in treating lung injuries. The potential of stem cells to develop into various cell types could facilitate the repair of damaged lung tissues, offering hope to patients with otherwise intractable conditions.
Moreover, advancements in biomaterials have introduced possibilities for lung scaffolding, allowing for engineered tissues that can mimic natural lung structure and support functionality. The uniqueness of regenerative medicine lies in its ability to establish long-term solutions rather than merely managing symptoms, which is often the case in traditional treatments. However, the field faces challenges, such as regulatory hurdles and the need for comprehensive clinical trials to validate safety and efficacy.
Frontiers in Lung Transplantation
Lung transplantation has made significant strides over the last few decades, yet numerous challenges remain. A recent exciting aspect of transplantation is the development of ex vivo lung perfusion (EVLP), a technique that allows for the evaluation and preservation of donor lungs outside the body. This advancement increases the viability of marginal donor lungs, expanding the donor pool and providing hope to patients on long waiting lists.
The essence of this innovation lies in its ability to improve outcomes for transplant recipients. However, with all new methods come risks—such as potential complications related to the procedure or rejection of the transplanted lungs. Addressing these concerns while maximizing patient benefits is a balancing act that continues to challenge researchers and clinicians alike.
"Research is the key to unlocking the future of lung health, paving the way for innovations that not only treat but also prevent diseases."
"Research is the key to unlocking the future of lung health, paving the way for innovations that not only treat but also prevent diseases."
By digging deeper into these areas, future research can not only bridge the gaps left by current knowledge but also pave new pathways for healthier lungs and lives. Tackling contemporary challenges will fortify the foundations upon which future explorations are built, ultimately catering to a more equitable and informed approach to lung health.
Concluding Remarks
In wrapping up the exploration of lung anatomy, it’s crucial to reflect on the holistic view that has been presented throughout this article. Each aspect, from structural nuances to functional dynamics, stitches together a rich tapestry of knowledge about the lungs that extends beyond mere description.
Understanding the anatomy of the lung isn't just an academic exercise; it has profound implications for health and disease management. The intricate design of the lungs allows for a myriad of functions, central to life itself. Recognizing how these structures operate provides a foundational understanding for future inquiries into respiratory health, potential interventions, and medical innovations.
"The lungs are not just organs; they are both the gateway to oxygen and a barometer of our overall well-being."
"The lungs are not just organs; they are both the gateway to oxygen and a barometer of our overall well-being."
As we delve into the specifics:
- The summary of key concepts we explored illustrates the critical roles of lung components.
- The implications for science and health underscore why ongoing research and understanding are vital for medical practices and treatment developments.
This concluding section serves as a reminder that the lungs, with their complex architecture and functions, play an indispensable role in our health. As we look to the future, the knowledge amassed here empowers both science enthusiasts and professionals to deepen their efforts in understanding and treating lung-related ailments, showcasing the relevance of this intricate organ system in broader health contexts.



