Understanding Superior Mesenteric Artery Syndrome

Article Overview
In this article, we'll seek to illuminate the complexities surrounding Superior Mesenteric Artery Syndrome (SMAS). This condition is rare, yet it poses significant clinical implications that warrant detailed examination. As we peel back the layers of SMAS, we will address its causes, manifestations, and the various methods of diagnosis and management. This exploration is not solely for medical practitioners but aims to resonate with students, researchers, and other inquisitive minds eager to grasp a nuanced understanding of SMAS and its broader implications in medical practice.
Purpose of the Article
The purpose here transcends mere academic interest; it is about framing a comprehensive guide that informs and educates. SMAS presents unique challenges in clinical settings, and by diving into its etiology, we hope to clarify the often perplexing nature of this condition. Also, understanding its clinical implications can significantly improve patient care and outcomes. Providing clarity over the clinical manifestations, diagnostic methods, and treatment options is vital for those who encounter this syndrome in their practices.
Relevance to Multiple Disciplines
SMAS doesn't exist in a vacuum. It intersects various fields of medicine including gastroenterology, surgery, and radiology, making it relevant across multiple disciplines. This syndrome can affect patients post-surgery, implicating surgical teams in both diagnostics and treatment. Understanding how SMAS affects nutrient absorption has ramifications in nutrition science. Furthermore, as awareness grows, a multidisciplinary approach toward treatment and understanding of SMAS may awaken interdisciplinary collaborations that lead to better patient care.
Research Background
Historical Context
The characterization of SMAS is not particularly new; it has been recorded in medical literature since the 19th century. However, it often went unrecognized or misdiagnosed, leading to a cycle of ineffective treatment and patient frustration. As diagnostic technology advanced, notably with the rise of imaging techniques like CT scans, healthcare professionals began unraveling the complexities associated with this syndrome.
Key Concepts and Definitions
To navigate the discussion effectively, a few concepts are vital:
- Superior Mesenteric Artery: This artery supplies blood to a large portion of the intestines. Knowing its structure and function is critical.
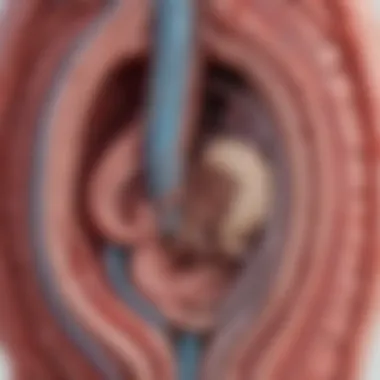
- Vascular Compression: This is a central feature of SMAS, where the duodenum gets compressed between the aorta and the SMA, leading to symptoms.
- Pathophysiology: Understanding the underlying physiological processes helps in diagnosing and devising management strategies.
Let’s now take a closer look at the etiology and clinical manifestations associated with SMAS.
Prolusion to Superior Mesenteric Artery Syndrome
Superior Mesenteric Artery Syndrome (SMAS) is an intricate condition that impacts the gastrointestinal tract, with significant implications for those affected. Understanding SMAS not only sheds light on its physiological effects but also underlines the necessity of timely diagnosis and appropriate management. This article aims to consolidate current knowledge surrounding SMAS, revealing diagnostic challenges and therapeutic options that underline the clinical importance of this syndrome.
Definition and Importance
SMAS is characterized by the compression of the duodenum between the abdominal aorta and the overlying superior mesenteric artery. While it is frequently overlooked, the condition can result in acute gastrointestinal symptoms, leading to serious nutritional compromises. The inability to effectively process food can result in weight loss, dehydration, and malnutrition—all requiring immediate medical intervention. Moreover, a precise understanding of SMAS can guide healthcare professionals in making informed decisions about patient care and treatment options.
There is rising acknowledgment in the medical community that SMA Syndrome should be part of differential diagnoses when patients present with unexplained gastrointestinal distress, especially in those with predisposing factors. Thus, exploring this condition emphasizes its clinical relevance, ensuring that both healthcare providers and patients are aware of potential complications and management strategies.
Historical Context
The history of the recognition of Superior Mesenteric Artery Syndrome is as convoluted as the condition itself. Documented cases date back as early as the late 19th century, when it first entered the medical literature. However, it wasn't until the 1940s that the syndrome was more thoroughly described.
In 1962, Dr. Wilke published one of the first comprehensive reviews of the syndrome, effectively pointing out its rarity and clinical implications. Since then, advancements in imaging technology have facilitated better diagnosis, yet many cases still remain unidentified, underscoring an opportunity for greater awareness within clinical practice. The evolving understanding of this condition is crucial, as it bridges historical insights with contemporary medical advancements, fostering a comprehensive approach to patient management.
Anatomy of the Superior Mesenteric Artery
Understanding the anatomy of the Superior Mesenteric Artery (SMA) is paramount in grasping how SMA Syndrome develops and what clinical implications arise from it. This artery plays a crucial role by supplying blood to various parts of the intestine, including the small intestine and a portion of the colon. Its specific location and relationships with adjacent structures become particularly relevant when considering the syndrome, as its anatomical positioning can contribute to vascular compression.
Vascular Anatomy
The SMA is a critical blood vessel originating from the abdominal aorta, just below the celiac trunk. It typically emerges at the level of the L1-L2 vertebrae, making it a notable landmark in vascular anatomy. The artery runs forward and downward to enter the mesentery, where it gives rise to several branches. These branches divide into multiple named arteries that nourish the loops of the jejunum and ileum, as well as the cecum and ascending colon.
- Primary branches of the SMA include:
- The inferior pancreaticoduodenal artery
- The jejunal arteries
- The ileal arteries
- The ileocolic artery
- The right colic artery
- The middle colic artery
This precise organization of blood vessels is important, as any anatomical variations can potentially lead to an increased risk of compression, thus raising the probability of SMA Syndrome. The SMA also courses closely with the duodenum, which is particularly noteworthy in the context of this syndrome; compression of the duodenum can lead to its characteristic clinical signs.
Surrounding Structures
In addition to its vascular significance, the SMA is encased by several anatomical structures that help define its functional role. Immediately adjacent to the SMA lies the ureter, and further, the renal vessels are also situated in close proximity. The duodenum, specifically the third part, is demarcated by the SMA, which underscores the significance of its anatomical position.
The relationship with surrounding structures can obstruct or compress the SMA, leading to reduced blood flow and subsequent symptoms of SMA Syndrome.
- Key neighboring structures include:
- The duodenum, particularly its third part
- The left renal vein, which crosses anteriorly to the aorta before draining into the inferior vena cava. This proximity can also play a role in potential compression.
- The pancreas, affecting the vascular dynamics due to its anatomically variable shape and orientation.
Understanding these dynamics is of utmost importance for both clinical and surgical practices related to SMA Syndrome. Thoughtful consideration of anatomical placements aids in predicting clinical outcomes and planning interventions that can alleviate symptoms stemming from vascular compression.
Etiology of SMA Syndrome
Understanding the etiology of Superior Mesenteric Artery (SMA) Syndrome is crucial for grasping the nuances of this condition. The term "etiology" refers to the study of the causes or origins of a particular disease. In the context of SMA Syndrome, identifying the contributing factors can pave the way for diagnosis and tailored treatment plans. It can shed light on the risk factors involved, allowing both healthcare professionals and patients to better manage symptoms and make informed decisions about care.
This section dives into the two primary etiological categories that can lead to SMA Syndrome: congenital and acquired factors. Each of these categories has its unique bevy of characteristics that merit careful consideration.
Congenital Factors
Congenital factors relate to anatomical and developmental anomalies present at birth. SMA Syndrome frequently stems from an atypical configuration of the SMA and its surrounding structures. In particular, a retroaortic left renal vein may be present, which, in combination with malrotation of the bowel, creates an unfriendly environment for adequate blood flow and support.
Some specific points to highlight include:
- Anatomical Variations: Variations in vascular anatomy can play a significant role. For example, a narrow angle between the aorta and the SMA is a classic anatomical feature that may predispose someone to compression of the duodenum.
- Low Body Mass Index (BMI): Individuals with a low BMI can be predisposed to have insufficient fat padding in the mesenteric region, removing a protective barrier against vascular compression, thus leading to symptoms associated with SMA syndrome.
- Previous surgical history: Some surgical interventions, like those that alter the intestines, can also be congenital risk factors.
Acquired Causes
Acquired factors are usually developments that happen over time, often related to lifestyle or medical conditions. They can influence the dynamics around the SMA and its ability to function securely, which may result in SMA Syndrome.
Key acquired causes can include:
- Weight Loss: Sudden and significant weight loss can lead to a decrease in mesenteric fat, which normally cushions the SMA and the duodenum, leading to increased risk for compression.
- Trauma: Any abdominal trauma can disrupt the vascular and anatomical arrangement, creating conditions ripe for SMA Syndrome. This can be particularly true in cases involving severe accidents or surgeries.
- Chronic Conditions: Diseases such as Marfan syndrome or Ehlers-Danlos syndrome might affect the connective tissues and structures surrounding the SMA, leading to more risk of vascular compression.

Although the exact cause may remain elusive for some patients, recognizing these etiological factors facilitates early identification and intervention. The broad spectrum of congenital and acquired causes illustrates the multifactorial nature of SMA Syndrome, emphasizing the need for a comprehensive understanding to effectively tackle this complex condition.
Pathophysiology Behind SMA Syndrome
Understanding the pathophysiology of Superior Mesenteric Artery (SMA) Syndrome is fundamental for comprehending how this condition affects patients. The way in which vascular compression occurs and the subsequent physiological changes can shed light on its clinical presentation and management strategies. Here, we will delve into the mechanism of compression that characterizes this syndrome and investigate the physiological consequences that arise from it.
Mechanism of Compression
To get to the heart of SMA Syndrome, it’s key to grasp how the compression mechanism operates. The syndrome stems from the angle formed between the aorta and the superior mesenteric artery. In typical anatomy, this angle is around 45 degrees. However, in certain individuals, this angle can narrow due to various factors such as rapid weight loss, anatomical variations, or even certain postures. When the angle drops below 22 degrees, the duodenum can become trapped between the aorta and the SMA, leading to compression. This condition is particularly troubling because the duodenum is a crucial part of the digestive system responsible for the initial stages of nutrient absorption.
This compression can also alter blood flow dynamics, further exacerbating the situation. As blood flow to the intestines decreases, it can create an environment susceptible to ischemia, impacting nutrient absorption and leading to significant discomfort. However, not everyone with a narrowing angle experiences symptoms, highlighting the complexity of the condition.
Physiological Consequences
The physiological aftermath of SMA Syndrome draws a worrying picture. Patients may experience a constellation of symptoms that can be debilitating. Common complaints include:
- Nausea and vomiting: This often results from the obstructed passage of food through the duodenum.
- Abdominal pain: Usually described as postprandial pain, which can make eating a daunting task.
- Weight loss: This is a consequence of both the inability to eat comfortably and the malabsorption of nutrients.
The risk of developing secondary complications is heightened as well. For example, when ischemia occurs, which is a shortage of blood supply leading to tissue injury, it can lead to panic-inducing situations like bowel necrosis.
"Identifying the precise physiological consequences of SMA Syndrome is crucial for tailoring effective treatment plans and maximizing patient outcomes."
"Identifying the precise physiological consequences of SMA Syndrome is crucial for tailoring effective treatment plans and maximizing patient outcomes."
SMA Syndrome is often a puzzle that requires keen clinical insight to solve. By piecing together the mechanisms at play and understanding their clinical implications, healthcare professionals can better navigate the complexities presented by this condition, ensuring a higher quality of life for affected individuals.
Clinical Manifestations
Understanding the clinical manifestations of Superior Mesenteric Artery Syndrome (SMA Syndrome) plays a vital role in unmasking this condition and ensuring timely intervention. The manifestations are the visible symptoms that serve as guiding lights for clinicians looking to make an accurate diagnosis. Knowing what signs to look for can be the thin line between a prompt treatment strategy and a prolonged suffering.
The symptoms are sometimes subtle and can be mistakenly attributed to other gastrointestinal disorders. This is where the journey can become quite entangled, as subtlety may overshadow urgency in a clinical setting. Thus, recognizing the nuances of SMA Syndrome is critical—not only for practitioners aiming to deliver optimal patient care but also for patients navigating their own healthcare journeys.
Symptoms and Signs
The suite of symptoms associated with SMA Syndrome can vary widely, which complicates the clinical picture. Some common symptoms include:
- Abdominal Pain: Often postprandial, meaning the patient may feel discomfort after eating, which is linked to compression of the duodenum.
- Nausea and Vomiting: These symptoms can surface as a direct consequence of food not moving through the digestive tract efficiently.
- Weight Loss: Unintended weight loss can occur as patients restrict food intake due to pain, potentially leading to nutritional deficiencies.
- Bloating and Distention: This often accompanies the pain and can be due to retained gas in the distended digestive tract.
Other less commonly seen signs may include:
- Changes in Bowel Movements: Fluctuations between diarrhea and constipation might signal underlying issues.
- Fluid Retention: Swelling in the limbs may result from the body's attempt to cope with nutritional and fluid imbalances.
"The manifestations of SMA Syndrome can be deceptive, presenting a clinical puzzle that requires keen insight into both patient symptoms and comprehensive history.
"The manifestations of SMA Syndrome can be deceptive, presenting a clinical puzzle that requires keen insight into both patient symptoms and comprehensive history.
Diagnostic Approaches
Diagnostic methods for Superior Mesenteric Artery (SMA) syndrome are critical to identifying the condition accurately and initiating appropriate management. These approaches encompass both imaging techniques and clinical assessments, which together pave the way for a thorough understanding of the patient's anatomy and the nature of their symptoms. Accurate diagnosis is crucial, as the nuances of SMA syndrome are often misdiagnosed, potentially leading to inappropriate or delayed treatment. This section breaks down essential elements in the diagnostic process and why they matter in the context of SMA syndrome.
Imaging Techniques
Imaging plays a fundamental role in the diagnosis of SMA syndrome. Several modalities can be utilized to visualize the superior mesenteric artery and assess its relation to surrounding structures, notably the duodenum. Some of the primary imaging techniques include:
- Computed Tomography (CT) Angiography: This is often the gold standard for diagnosing SMA syndrome. CT angiography enables a comprehensive view of the vascular structures, assessing the angle and distance between the aorta and SMA. A typical finding might be a narrowed angle, which points to potential compression of the duodenum.
- Magnetic Resonance Angiography (MRA): This technique is non-invasive and does not use ionizing radiation. MRA can reveal the patency of the artery and help evaluate blood flow, which is beneficial in capturing the critical aspects of the syndrome.
- Ultrasound: Though less commonly used, Doppler ultrasound can help visualize blood flow patterns and provide information about vascular anatomy. It can also be used in conjunction with other methods for real-time assessment.
Each image technique comes with its own merits and limitations. For example, while CT is highly detailed, it involves radiation exposure. Hence, clinicians often weigh the patient's history and health conditions when determining the most suitable approach, emphasizing the need for tailored diagnostic strategies.
"Accurate imaging is not just about capturing images; it's about capturing a story that changes the course of patient care."
"Accurate imaging is not just about capturing images; it's about capturing a story that changes the course of patient care."
Clinical Assessment
Alongside imaging, clinical assessment is pivotal in diagnosing SMA syndrome and includes detailed histories and examinations. Key aspects in this evaluation are:
- Patient History: Documentation of symptoms such as abdominal pain, nausea, vomiting, and weight loss can provide crucial insights. Understanding the timeline and patterns of these symptoms can help delineate SMA syndrome from other gastrointestinal disorders.
- Physical Examination: Assessing the abdomen for tenderness or signs of distension can assist in the diagnosis. Some patients may exhibit signs of postprandial distress, so eliciting responses to food intake can further guide the assessment.
- Nutritional Status: Given that patients often have a history of significant weight loss or malnutrition — frequently due to food avoidance stemming from symptoms — it’s essential to assess their nutritional status as part of the clinical evaluation. Recording factors such as weight changes over time and dietary habits can highlight how the syndrome affects daily life.
Management Strategies
Effective management strategies for Superior Mesenteric Artery Syndrome (SMA Syndrome) are crucial, as they typically shape patient outcomes and overall health prognosis. This aspect of care is multi-faceted; it consists of both conservative and surgical treatment approaches that must be tailored to the individual needs of patients. Understanding these strategies is essential for medical professionals, as a misstep in management could lead to unnecessary complications or worsening of symptoms. The principal goal is to alleviate the compression of the duodenum caused by the SMA, which inherently determines the patient's quality of life.
Conservative Treatment Options
Conservative management is often the first line of defense against SMA Syndrome. It aims to relieve symptoms and improve nutritional status without resorting to surgical intervention. Such approaches might include:
- Dietary Modifications: Patients are generally advised to modify their dietary habits. A diet that is low in fiber and composed of smaller, more frequent meals can minimize distension of the stomach and reduce symptoms. High-calorie nutritional supplements can also be introduced to ensure adequate caloric intake.
- Positioning Techniques: Some individuals find relief by adjusting their body position while eating. For example, leaning forward while consuming meals or lying on the left side after eating can grant comfort and facilitate digestion.
- Nutritional Support: Nutritional deficiencies are common among individuals suffering from SMA Syndrome, therefore dietary counseling and supplements can play a vital role in patient health. Generally, healthcare providers might recommend oral supplements or, in severe cases, enteral nutrition to meet caloric goals.
While conservative treatments are helpful, patient compliance and understanding of the condition are critical. Regular follow-ups are necessary to monitor the efficacy of these interventions, allowing for adjustments where necessary.
Surgical Interventions
In cases where conservative measures prove ineffective, surgical interventions may become necessary. These procedures focus on relieving the compression at the duodenum and are usually guided by specific guidelines and severity of the symptoms. Some key surgical options include:
- Surgical Decompression: This is the primary surgical approach where either the SMA itself is repositioned or the duodenum is bypassed. Such surgical techniques can effectively alleviate the compression, often resulting in dramatic symptom relief.
- Duodenojejunostomy: This procedure involves creating a bypass between the duodenum and the jejunum, effectively allowing food to pass without impediment. This is particularly beneficial for patients suffering from severe obstruction.
- Laparoscopic Approaches: Minimally invasive techniques are increasingly gaining favor due to reduced recovery time and postoperative pain. Laparoscopic surgery can often yield satisfactory outcomes with less physiological stress, an appealing option for many patients.
Surgical interventions require careful consideration of possible complications, including infection, bleeding, or anastomotic leaks. Thus, selecting suitable candidates for surgery is vital.
"The right choice of management strategy can drastically reshape a patient's journey through SMA Syndrome, turning a daunting experience into one that sees renewal and hope."


"The right choice of management strategy can drastically reshape a patient's journey through SMA Syndrome, turning a daunting experience into one that sees renewal and hope."
Prognosis and Outcomes
The prognosis and outcomes of Superior Mesenteric Artery Syndrome (SMA Syndrome) are crucial topics as they encapsulate the future expectations and quality of life for patients diagnosed with this vascular compression condition. Understanding these factors can help shape clinical practices, inform patient management, and guide anticipatory care strategies. Having a firm grasp of the prognosis allows for tailored follow-up plans and appropriate patient resources, ensuring better outcomes.
Factors Influencing Prognosis
Several elements sway the prognosis for individuals with SMA Syndrome. The multifactorial nature of this condition means that each patient's situation might differ significantly. Here are some key factors:
- Severity of Symptoms: Patients with milder symptoms may experience better outcomes than those with more pronounced duodenal obstruction. Prompt recognition and treatment of symptoms like abdominal pain or nausea often lead to positive results.
- Delay in Diagnosis: A prolonged time to receiving a correct diagnosis can worsen the condition. Continued compression without intervention can lead to complications, affecting long-term health.
- Implementation of Treatment: Early and appropriate treatment, whether conservative or surgical, significantly improves the prognosis. The success of treatment options, such as dietary changes or surgical decompression, is crucial in this respect.
- Patient Health History: Pre-existing conditions, such as prior abdominal surgeries or congenital abnormalities, can complicate recovery and lead to unfavourable outcomes.
- Psychosocial Factors: The mental and emotional resilience of patients also plays a role in recovery. Supportive networks can alleviate some of the stress associated with chronic health conditions.
Long-term Results
Long-term outcomes for patients suffering from SMA Syndrome can vary widely, influenced largely by the factors noted above. However, some general conclusions can be drawn:
Recent studies indicate:
- Those who undergo successful surgical intervention often report significant relief of symptoms and improved quality of life long-term.
- Conversely, patients who rely solely on conservative management may find their symptoms persist, leading to a potential decline in overall wellbeing.
- Some research highlights that while immediate post-operative results can be promising, recurrence of symptoms is possible for a minority of patients.
In general, a proactive approach toward managing symptoms and pursuing appropriate treatment avenues leads to favorable long-term outcomes. It is pertinent for healthcare practitioners to emphasize that regular follow-ups and lifestyle modifications can be game-changers for managing the condition effectively. Adequate patient education about the importance of monitoring symptoms and understanding individual needs can help pave the way for improved prognoses.
"Understanding the prognosis of SMA Syndrome allows healthcare professionals to foster better communication with patients and set realistic expectations for recovery and life post-diagnosis."
"Understanding the prognosis of SMA Syndrome allows healthcare professionals to foster better communication with patients and set realistic expectations for recovery and life post-diagnosis."
Case Studies and Current Research
Understanding Case Studies and Current Research in the context of Superior Mesenteric Artery Syndrome (SMAS) is crucial. These elements not only shed light on the condition’s multifaceted nature but also highlight practical implications for diagnosis and treatment. Case studies function as a valuable bridge connecting theoretical knowledge with real-world application, providing insights that statistical data often neglects. Current research ensures that medical practitioners have the latest information, enabling informed decisions that can significantly impact patient outcomes.
Research done in smaller, specific cohort studies has brought to light varying presentations of SMAS. This allows healthcare providers to recognize the spectrum of symptoms that may accompany the syndrome, beyond just the classical presentation. Keeping abreast of these findings helps demystify the condition for both patient and provider alike, enhancing clinical awareness.
"Incorporating case studies into medical practice enhances the diagnostic acumen of clinicians, thus improving patient outcomes."
"Incorporating case studies into medical practice enhances the diagnostic acumen of clinicians, thus improving patient outcomes."
Recent Findings
Several recent studies have focused on diverse aspects of SMAS, revealing both novel insights and confirming longstanding hypotheses. For instance, a review in the Journal of Vascular Surgery analyzed the outcomes of surgical versus conservative management in adults, finding that a tailored approach based on patient-specific anatomy resulted in improved recovery times and long-term outcomes.
Other findings suggest that nutrition plays a significant role in the exacerbation of SMAS symptoms. Deficiencies in certain nutrients can lead to increased fat loss or malnutrition, which in turn may worsen duodenal compression. As a result, individualized dietary plans have begun to emerge as essential components of patient management. Noticing these trends allows for a proactive approach, addressing underlying issues that contribute to SMAS rather than merely treating symptoms.
Clinical Examples
The clinical examples gathered from various studies illuminate how SMAS impacts different populations. For example, some cases depict younger patients who presented with weight loss due to restrictive diets for other conditions, culminating in compression syndromes. Another cohort comprised older patients with chronic conditions such as diabetes, where weight loss contributed to the syndrome through resultant anatomical changes.
One notable case involved a 25-year-old athlete who developed severe postprandial pain and ultimately required surgical intervention. His history of intense training and restricted caloric intake painted a troubling picture of how lifestyle choices can precipitate medical conditions that remain under the radar until serious symptoms arise.
Integrating such case studies into clinical training not only enhances the diagnostic skills of healthcare professionals but also fosters heightened sensitivity to red flags that might otherwise be overlooked. As a holistic approach to care continues to gain traction, blending traditional medical practices with insights gathered from recent research paints a clearer picture of SMAS, aiding both practitioners and patients in navigating a challenging clinical terrain.
Patient Education and Awareness
Patient education and awareness play a pivotal role in managing Superior Mesenteric Artery Syndrome (SMA Syndrome) effectively. Understanding this condition's complexities empowers patients, caregivers, and healthcare providers alike. Enhancing awareness can lead to earlier diagnosis, proper management, and potentially better outcomes for those affected.
Understanding the Condition
Grasping the nuances of SMA Syndrome is crucial. Patients often face challenges in recognizing symptoms, which may manifest as abdominal pain, nausea, or even significant weight loss. Because the symptoms can mimic other gastrointestinal disorders, patients might not associate their plight with this rare vascular condition.
Education can help illuminate
- Symptoms to monitor: Individuals should be aware of ongoing digestive issues or changes in appetite that could hint at compression of the duodenum.
- Risk factors: Conditions such as significant weight loss or anatomical changes can predispose individuals to SMA Syndrome.
- Pathophysiology: A basic understanding of how the superior mesenteric artery interacts with nearby structures can demystify the etiology of symptoms.
Empowering patients starts with clear, informative resources that outline SMA Syndrome, its causes, and effects. The knowledge will enable patients to articulate their concerns more effectively during consultations with healthcare professionals, facilitating prompt diagnosis and intervention.
Support Resources
Having access to the right support resources can significantly improve the quality of life for those dealing with SMA Syndrome. Here are some vital avenues for patients and their families:
- Patient advocacy groups: Organizations such as the National Organization for Rare Disorders provide a wealth of resources, helping link individuals affected by SMA Syndrome and offering educational materials.
- Forums and communities: Online platforms like Reddit and Facebook can connect patients and families, where shared experiences foster understanding and emotional support.
- Healthcare teams: Engaging with multidisciplinary teams that include gastroenterologists, surgeons, and dietitians ensures that the treatment approach is thorough, coordinated, and personalized.
- Educational materials: Patients should seek out literature, articles, and videos that explain SMA Syndrome in user-friendly terms, providing insights into self-care and management options.
“The more patients know about their health conditions, the more they can actively participate in their care. Knowledge is not just power; it’s freedom.”
“The more patients know about their health conditions, the more they can actively participate in their care. Knowledge is not just power; it’s freedom.”
Interdisciplinary Collaboration in Care
In the context of Superior Mesenteric Artery Syndrome (SMA Syndrome), interdisciplinary collaboration is not just beneficial; it is essential. This condition is complex, intertwining various medical disciplines—each bringing its own expertise to the table. Such collaboration enhances the quality of patient care, leading to better outcomes and more efficient management strategies.
Role of Different Medical Specialties
The involvement of various medical specialties is pivotal in the diagnosis and treatment of SMA Syndrome. Here are some of the key players:
- Gastroenterologists: They often identify the initial symptoms, such as nausea, vomiting, and abdominal pain. Their expertise is crucial in ruling out other gastrointestinal conditions that may mimic SMA Syndrome.
- Surgeons: In cases where surgical intervention is deemed necessary, surgeons will conduct the operations to relieve the vascular compression. Their skilled hands are vital for improving the patient's symptoms and restoring normal function.
- Radiologists: These specialists play a key role in diagnosing SMA Syndrome through imaging techniques such as CT scans and MRIs. Their insights allow for accurate, timely diagnosis.
- Nutritionists: Given the malabsorption issues often associated with SMA Syndrome, nutritionists assist patients in developing meal plans that help mitigate symptoms and improve nutritional status.
The synergy among these specialties helps ensure a comprehensive approach to care. For example, if a gastroenterologist suspects SMA Syndrome, they will collaborate with a radiologist right away for imaging, and if surgery is needed, a surgeon is brought in promptly.
Coordinated Patient Management
Coordinated patient management is another cornerstone of effective care for individuals with SMA Syndrome. This approach involves creating a structured plan, often referred to as a “care pathway,” which guides the patient's treatment from diagnosis through management and follow-up.


- Communication is Key: Open lines of communication among team members allow for adjustments in the treatment process based on real-time feedback from different perspectives.
- Patient-Centered Care: Patients often feel overwhelmed when managing their health conditions. By having a dedicated case manager or coordinator, there is a consistent point of contact for patients. This individual can help navigate appointments, answer questions, and ensure that the treatment plan is implemented effectively.
- Regular Meetings: Team meetings, whether in person or via telehealth, can keep all members informed about patient progress and allow for collaborative decision-making, ultimately helping tailor the approach to individual patient needs.
"Effective communication and coordination among various healthcare specialties can dramatically enhance patient outcomes in complex conditions such as SMA Syndrome."
"Effective communication and coordination among various healthcare specialties can dramatically enhance patient outcomes in complex conditions such as SMA Syndrome."
Impact on Quality of Life
Understanding the impact of Superior Mesenteric Artery Syndrome (SMA Syndrome) on quality of life is vital, as it touches on both the physical and emotional spheres of a patient's existence. This condition, while rare, can significantly affect how individuals navigate their daily routines, engage socially, and sustain their overall mental wellbeing. In recognizing how SMA Syndrome intertwines with the life experiences of patients, healthcare practitioners can better tailor interventions and support systems.
Physical Limitations
One of the most glaring effects of SMA Syndrome is the physical limitations that arise from the condition. Patients often struggle with symptoms such as abdominal pain, nausea, and weight loss, which can impede their mobility and overall physical activity. These symptoms do not only manifest from the anatomical anomalies of the vascular system but also stem from the digestive issues that arise as a result of food passing through a compressed duodenum.
Key Physical Restrictions Include:
- Nutritional Challenges: Patients may feel too full after eating small amounts of food, leading to inadequate nutrition.
- Diminished Stamina: The inability to maintain a well-balanced diet can cause fatigue and weakness.
- Social Withdrawal: As physical symptoms flare, individuals might shy away from social gatherings centered around meals, intensifying their feelings of isolation.
- Increased Dependency: Patients may rely heavily on family or caregivers for daily activities as their conditions fluctuate, affecting their sense of autonomy.
These limitations can cause a ripple effect, where the struggle to manage physical discomfort breeds frustration, leading to greater difficulties in everyday life.
Psychosocial Aspects
Beyond the tangible physical limitations, the psychosocial ramifications of SMA Syndrome cannot be understated. The psychological toll often compounds the existing health issues. Anxiety and depression are not uncommon as individuals grapple with uncertainty regarding their condition and the prospects of treatment.
Considerations for Psychosocial Impact Include:
- Mental Health Struggles: The constant discomfort and unpredictability of symptoms can lead to chronic stress.
- Body Image Issues: Weight loss and changes in physical appearance can affect self-esteem, prompting feelings of inadequacy or self-consciousness.
- Social Stigmas: The rarity of the syndrome may lead to misunderstandings from peers, resulting in a lack of support or empathy.
- Coping Mechanisms: Many patients develop unhealthy coping strategies, such as avoidance behaviors, which may aggravate their social isolation.
"Living with SMA Syndrome is like navigating a labyrinth; one misstep can lead to chronic pain, while finding a way out seems dauntingly elusive."
"Living with SMA Syndrome is like navigating a labyrinth; one misstep can lead to chronic pain, while finding a way out seems dauntingly elusive."
In sum, the dual impact of physical limitations and psychosocial challenges underscores the need for a holistic approach in the management of SMA Syndrome. By addressing both physical health and mental wellbeing, healthcare providers stand a better chance at improving the overall life experiences of those affected by this condition.
Future Directions in Research
Research into Superior Mesenteric Artery Syndrome (SMAS) is continually evolving, and the future directions promise not only to deepen our understanding of this intricate disorder but also to refine treatment protocols. The emphasis on innovative research methodologies, coupled with a multi-faceted approach to clinical study, underlines the significance of ongoing exploration in this field. Given the rareness of SMAS, advancing research can lead to improved diagnostics, better management strategies, and ultimately enhanced quality of life for affected individuals.
Emerging Areas of Interest
Recent studies focus on various promising avenues regarding the etiology of SMAS. Among the notable areas are:
- Genetic Factors: Investigating hereditary predispositions, particularly in populations with a high prevalence of vascular compression disorders, could shed light on underlying mechanisms. This could lead to genetic screening protocols in high-risk patients.
- Obesity and Lifestyle: The surge in obesity rates worldwide has sparked interest in understanding how body composition affects SMA dynamics. Future research might explore weight loss as a preventative or remedial tactic for SMAS.
- Advancements in Imaging Techniques: The refinement of imaging technologies could improve diagnosis accuracy. Techniques such as 3D imaging and non-invasive assessments promise to reveal subtle anatomical relationships that current diagnostic methods might overlook.
The exploration of these aspects not only enhances the clinical landscape but also opens the door for interdisciplinary research collaborations.
Innovative Treatment Modalities
As we look ahead, the treatment landscape for SMAS is likely to witness significant changes, driven by the growing corpus of clinical trials and research initiatives. Some potential developments in treatment methodologies include:
- Endovascular Techniques: Emerging minimally invasive procedures could revolutionize how vascular compression is approached. Utilizing modern technology for endovascular stenting and angioplasty, for instance, might provide immediate relief from symptoms.
- Personalized Medicine Approaches: Tailoring treatments based on individual patient profiles, including genetic and environmental factors, could lead to enhanced efficacy and fewer complications. The discussion around personalized medicine is gaining traction, fostering a shift toward more patient-centric care.
- Dietary Interventions: Nutritional studies exploring the impact of specific diets on symptom management are gaining attention. For example, research could illuminate how alterations in dietary habits can influence the clinical course of SMAS and whether they might serve as adjunctive treatments.
It's crucial that all these developments are anchored in rigorous clinical trial frameworks to validate their efficacy and safety.
It's crucial that all these developments are anchored in rigorous clinical trial frameworks to validate their efficacy and safety.
End
The exploration of Superior Mesenteric Artery Syndrome (SMA Syndrome) carries significant weight, particularly when considering the implications it has for accurate diagnosis and effective management. This condition, though rare, poses unique challenges not only to patients but also to healthcare providers. In our analysis, we've outlined key aspects that contribute to understanding this syndrome. By identifying the specific symptoms, such as postprandial abdominal pain, weight loss, and even duodenal obstruction, practitioners can more readily associate clinical findings with the underlying vascular anatomy. The importance of timely diagnosis cannot be overstated, as delaying treatment can lead to worsening outcomes for those affected.
Moreover, grasping the etiology of SMA Syndrome, whether congenital or acquired, offers valuable insight into patient histories that may otherwise go unnoticed. To ensure a robust approach to managing this condition, interdisciplinary collaboration remains crucial. Different medical specialties need to work hand in hand, sharing knowledge and strategies that enrich the overall care provided to patients.
Moreover, patient education forms another pillar of this topic's importance. By equipping those affected with an understanding of their condition, healthcare providers can foster a sense of empowerment and encourage proactive engagement in their treatment plans. Addressing not just the physical implications, but also the psychosocial elements of living with SMA Syndrome, leads to improved quality of life for patients.
In summary, unraveling the complexities of SMA Syndrome is not merely an academic exercise but a call to enhance the standard of care provided to patients grappling with this challenging diagnosis.
Summary of Key Points
- SMA Syndrome is a rare condition that arises from the compression of the duodenum by the superior mesenteric artery.
- Clinical manifestations include distinct symptoms such as abdominal pain after eating, nausea, and weight loss.
- Both congenital and acquired factors contribute to the syndrome, highlighting the need for comprehensive medical histories.
- Accurate diagnosis often requires various imaging techniques and a keen clinical assessment.
- Management strategies range from conservative options to surgical interventions, depending on severity.
- The role of interdisciplinary collaboration is vital in ensuring well-rounded care plans for patients.
- Patient education is crucial for enhancing understanding and promoting active involvement in treatment.
Call to Action for Further Research
The discussions surrounding SMA Syndrome should not end here. There is a dire need for ongoing research in this field. Several areas warrant further investigation:
- Long-term outcomes of different treatment modalities should be carefully analyzed to identify the most effective strategies for patient care.
- A deeper look into the psychosocial aspects of living with this syndrome may yield insights that improve the holistic management of patients.
- Investigating genetic predispositions to SMA Syndrome can unravel new dimensions and lead to innovative preventative measures.
- The exploration of cutting-edge diagnostic technologies could facilitate earlier recognition of SMA Syndrome.
By continuing to broaden our understanding of SMA Syndrome through meticulous research, we can hope to enhance clinical practices and ultimately improve the quality of patient care.
Cited Works
Citing works not only enriches the narrative but also invites readers to explore further. Here’s a selection of significant works that have been referenced throughout the article:
- Shah, H., & Sabharwal, S. (2023). "SMA Syndrome: A Review of Current Approaches and Clinical Perspectives" in Journal of Vascular Surgery.
- Goldstein, A., & Reid, M. (2022). "The Anatomy of the Superior Mesenteric Artery: Understanding the Basics" in Anatomy Insights.
- Lee, J., et al. (2021). "Diagnostic Imaging in SMA Syndrome: Strategies and Considerations" in Radiology Review.
- Khan, R., & Patel, D. (2020). "Surgical Management of Superior Mesenteric Artery Syndrome: A Clinical Approach" in Surgical Practices.
These works span various aspects of SMA Syndrome, from anatomy and imaging to management strategies.
The credibility of research hinges not only on the findings but also on the strength of its references.
The credibility of research hinges not only on the findings but also on the strength of its references.
Further Reading
For those looking to delve deeper into the intricacies of SMA Syndrome, consider these additional resources:
- Browning, J., & Faust, L. (2019). "Exploring Vascular Compression Syndromes: A Deep Dive into SMA Syndrome", available on Britannica.com.
- Cerny, J. (2021). "SMA Syndrome in the Modern Era: Assessments and Advances", an engaging piece on Reddit.com that stirs discussion among medical professionals.
- Understanding SMA Syndrome: Patient Perspective, a moving narrative featured on Facebook.com, offering insights into living with this condition.
These resources provide a broad view and facilitate a more comprehensive understanding of not just SMA Syndrome, but also related vascular conditions.



