Understanding the Sacral Spine: Anatomy and Health

Article Overview
The sacral spine serves as a vital part of human anatomy, often overlooked in mainstream discussions about spinal health. Understanding its structure and functions can provide insights into various clinical conditions that affect not just the spine itself but also overall bodily health.
Purpose of the Article
The aim of this article is to shed light on the complexity and significance of the sacral spine. We will dissect its anatomy and biomechanics, exploring how it contributes to physiological functions including mobility, stability, and load distribution. Additionally, it will delve into common disorders related to the sacral region, discussing treatments and preventive measures.
Relevance to Multiple Disciplines
This discourse on the sacral spine is crucial for healthcare professionals such as physical therapists, chiropractors, and orthopedic surgeons, who often interact with conditions stemming from the sacral area. Furthermore, students of anatomy, physiology, and related fields will find this article rich in detail, aiding in their understanding of interconnectivity within the human body. Even those outside the medical field may gain valuable insights into how the structure they might take for granted influences their daily life.
Research Background
Historical Context
Historically, the sacral spine was often seen as a passive structure, merely serving to connect the spine to the pelvis. However, advancements in medical imaging and biomechanics have transformed our understanding, revealing its dynamic role in movement and posture. From the initial descriptions in ancient anatomy texts to contemporary research that ties sacral function to various conditions (e.g., lower back pain), the narrative around the sacral spine has evolved significantly.
Key Concepts and Definitions
Understanding certain terminologies is fundamental to grasping the content that follows.
- Sacrum: A triangular bone at the base of the spine, made up of five fused vertebrae. It connects the spine to the hip bones.
- Sacral Nerves: Nerves that emerge from the sacral plexus, influencing both sensation and movement in the lower body.
- Biomechanics: The study of the mechanical laws relating to the movement or structure of living organisms, providing insights into how the sacral spine interacts with other spinal regions.
By laying this groundwork, we can better appreciate the implications of sacral spine health and its interconnectedness within the human body.
"The sacral spine is not just an anatomical structure; it's a hub of functionality that influences how we move through life."
"The sacral spine is not just an anatomical structure; it's a hub of functionality that influences how we move through life."
As we continue this exploration, the sections to follow will dive deeper into the sacral spine's specific anatomy and the clinical implications that arise from its study.
Prolusion to the Sacral Spine
The sacral spine, often overshadowed by the more commonly discussed cervical and lumbar regions, holds a critical position in understanding human anatomy and functionality. It is not merely a collection of bones; rather, the sacral spine embodies a complex interplay of structural stability, biomechanical function, and neural integration. In this section, we will delve into the intricacies of this anatomical marvel, highlighting its significance not just in terms of anatomy, but its broader implications for health, movement, and rehabilitation.
Significance of the Sacral Spine in Human Anatomy
The sacral spine comprises five fused vertebrae, forming a triangular structure at the base of the vertebral column. This unique positioning enables it to act as the keystone in pelvic stability and support. The sacrum connects the spine to the pelvis, clearly indicating its vital role in maintaining balance and facilitating movement. This region houses critical nerves that contribute to sensations and motor functions in the lower limb, highlighting the potential for a cascade of issues when dysfunction occurs.
Understanding the sacral spine integrates knowledge across various disciplines: anatomy, biomechanics, and even physical therapy.
Moreover, injuries or conditions affecting the sacral region can lead to significant limitations in mobility and quality of life. Therefore, recognizing its importance in our overall anatomy enables medical professionals to make informed decisions about evaluation and treatment.
Overview of Sacral Anatomy
Taking a closer look at sacral anatomy reveals its layered complexity. The sacrum, comprised of sacral vertebrae, fuses into a single bone after adolescence. This fused configuration adds strength and stability, supporting the weight of the upper body and distributing it evenly to the pelvis.
The shape of the sacrum is not arbitrary; its wedge-like structure allows for the optimal distribution of forces during movement, such as walking or lifting. Each side of the sacrum articulates with the ilium to form the sacroiliac joints, establishing critical connections between the spine and pelvis.
In addition to the robust framework, the sacral canal serves as a conduit for the sacral nerve roots. Numerous foramina line the sacrum, providing exit points for these nerves to innervate the lower body. This exit is essential for overall function, as issues in this region can lead to pain, numbness, or weakness in the legs.
"The sacral spine's role in facilitating movement and maintaining balance cannot be overstated. Understanding its anatomical nuances is crucial for effective diagnosis and treatment of related disorders."
"The sacral spine's role in facilitating movement and maintaining balance cannot be overstated. Understanding its anatomical nuances is crucial for effective diagnosis and treatment of related disorders."
In summary, the sacral spine is a fundamental component of human anatomy, with broad implications for movement, stability, and health. By examining its structure and significance, we set the stage for deeper exploration of its functionality, common disorders, and potential treatment strategies.
Anatomical Features of the Sacral Spine
Understanding the anatomical features of the sacral spine serves as a linchpin in grasping its vital functions and clinical significance. The sacrum may seem like a mere wedge of bone tucked away at the base of the spine, but its complexity is worthy of deeper exploration. It operates as a keystone, holding the entire structure of the pelvis together while also interacting seamlessly with surrounding anatomical structures.
Structure of the Sacrum
The sacrum is a unique triangular bone made of five fused vertebrae, often numbered S1 to S5. Its design resembles a shield, which provides not only support but also stability to the pelvis. This fusion transforms the sacrum into a robust platform, assisting weight transfer from the spine to the lower limbs.
The sacrum articulates with the lumbar vertebrae above and the coccyx below, forming several joints, which include the lumbosacral joint and the sacrococcygeal joint. Moreover, the boundaries of the sacrum are marked by the sacral promontory at the anterior superior edge, aiding in defining its anterior aspect. It’s no ordinary bone; its anatomical configuration is an ingenious adaptation to mechanical stresses imparted during activities like walking and running.
Vertebral Composition
In terms of vertebral composition, the sacrum includes specialized structures that further clarify its purpose. The vertebrae's unique characteristics contribute significantly to the overall biomechanics of the spine. For instance, the sacral vertebrae possess broad, thick bodies which allow for bearing greater loads compared to their cervical or lumbar counterparts.
Each sacral vertebra features transverse processes that extend laterally, which serve as attachment points for ligaments and muscles. They also contain sacral foramina, small openings that permit the passage of sacral nerves and blood vessels, ensuring sufficient neural and vascular supply to the pelvic region. This anatomical alignment plays a crucial role in functional stability, allowing the sacrum to act as a fulcrum for pelvic and lower limb movements.
Sacral Canal and foramina
The sacral canal deserves a mention for its importance in spinal health. It runs through the center of the sacrum and houses the spinal nerves, which branch out through the sacral foramina. These openings provide crucial exits for the nerves that innervate not only the lower extremities but also organs within the pelvic cavity.
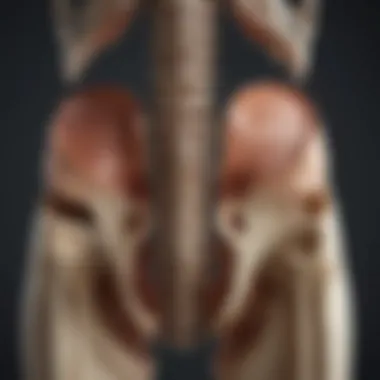

The configuration of these foramina is purposeful; it allows for flexibility and mobility while still protecting the nerve roots from injury. The sacral canal narrows as it descends, forming the sacral hiatus, another key anatomical feature through which the filum terminale extends.
"The sacral canal is not merely a passage; it's a vital highway for nerve communication between the spine and the lower body."
"The sacral canal is not merely a passage; it's a vital highway for nerve communication between the spine and the lower body."
These anatomical nuances surrounding the sacral spine reveal it as more than just a structural vestige. Its complex architecture signifies a dynamic interplay between biology and function, imperative for maintaining human posture, gait, and pelvic stability. Grasping these features lays a solid foundation for understanding the functional and clinical dimensions of the sacral spine in both health and disease.
Functionality of the Sacral Spine
The functionality of the sacral spine is a cornerstone of understanding both its role in the human body and its clinical significance. The sacrum serves as the keystone of the pelvic architecture, supporting weight mechanisms between the upper body and the lower limbs. In doing so, it plays a key role in various physical activities and contributes to overall mobility. Understanding how the sacral spine operates is critical, particularly in fields such as physical therapy, sports medicine, and rehabilitation.
Biomechanics of the Sacral Region
The biomechanics of the sacral region are fascinating, as this area essentially acts as a bridge between the spine and the pelvis. The sacrum is uniquely positioned to manage loads and stress distributed from the body above it and those from the lower limbs. When considering the forces at play, it's essential to highlight the sacrum’s triangular shape. This anatomical feature helps distribute weight efficiently throughout the pelvis, supporting activities ranging from standing to high-impact sports.
During walking or running, the sacral region absorbs a significant amount of the impact forces. The lumbosacral junction (where the lumbar spine meets the sacrum) acts as a fulcrum for movement, allowing for a proper balance between stability and flexibility. In many ways, the sacral spine is like a well-tuned engine, running efficiently under the right circumstances but easily thrown out of whack by factors such as poor posture or injury.
For instance, when someone carries excessive weight, they can inadvertently shift the load unevenly, causing stress on the sacral region, which may lead to discomfort or injury.
Role in Pelvic Stability
Pelvic stability hinges on the sacral spine, proving crucial when it comes to functions that require core strength and balance. The sacrum connects with the ilium bones via the sacroiliac joints, creating a solid base that allows force to be transferred during movement. Without this robust connection, your ability to perform basic tasks—like walking or sitting upright—would be significantly impaired.
The relationship between the sacral spine and the pelvic floor muscles deserves attention, too. These muscles work in tandem to provide stability. When the pelvic floor is strong, the sacral spine can better support the body and maintain posture. Weakness in this area may lead to issues such as pelvic instability or lower back pain. In clinical settings, assessing pelvic stability is crucial when devising treatment plans for individuals suffering from related disorders.
Nervous System Interactions
The sacral spine is not just a structural component; it’s also pivotal in communicating with the nervous system. The sacral vertebrae house spinal nerves responsible for innervating key areas, particularly those controlling lower limb function and pelvic organs. Dysfunction or injury within the sacral spine can manifest as neurological symptoms, such as pain radiating down the legs or issues with bowel and bladder control.
This interactivity between the sacral region and nervous system underscores why disorders of the sacrum can lead to varied and complex clinical presentations. A thorough understanding of these interactions is essential for practitioners in diagnosing and treating conditions affecting the sacral spine. Implementing appropriate imaging techniques and physical examination methodologies can shed light on such issues, allowing for targeted interventions.
The sacral spine serves both as a structural and functional hub, integral to various systems within the body.
The sacral spine serves both as a structural and functional hub, integral to various systems within the body.
End
The functionality of the sacral spine is multifaceted. From biomechanics to stability roles and nervous system interactions, this area deserves more than just cursory acknowledgment in anatomical studies. By appreciating the complexities of the sacral spine's functionality, healthcare professionals can make informed decisions that enhance treatment outcomes and improve quality of life for patients.
Common Conditions Affecting the Sacral Spine
Understanding the common conditions affecting the sacral spine is paramount for both healthcare providers and patients alike. These conditions can not only impair quality of life but also lead to complex clinical challenges. The sacrum, a critical component of the lower spine, serves as a nexus between the spine and pelvis, carrying significant weight and responding to mechanical stresses.
Awareness of these common issues allows for timely intervention, lessening the burden of pain and dysfunction. Moreover, this knowledge is vital for facilitating early diagnosis and management, which ultimately leads to improved outcomes for those affected.
Sacral Fractures
Sacral fractures often arise from a traumatic event such as falls, motor vehicle accidents, or sports injuries. They may not always be immediately apparent, as symptoms can manifest ambiguously. Individuals may experience localized pain, particularly during movements like standing, sitting, or even during coughing. It is crucial to understand how these fractures can disrupt normal function and potentially lead to chronic conditions if left unattended.
"Sacral fractures can behave like hidden monsters, lurking beneath the surface, making diagnosis a tricky endeavor."
"Sacral fractures can behave like hidden monsters, lurking beneath the surface, making diagnosis a tricky endeavor."
Key considerations include:
- Risk of further injury: Untreated fractures can lead to instability and further damage to surrounding structures.
- Potential for nerve involvement: In severe cases, the fracture can impact nerve roots leading to numbness or weakness in the legs.
Imaging techniques, including X-rays and MRIs, are essential for accurately diagnosing these fractures, guiding treatment decisions effectively. In many instances, conservative management such as rest and physical therapy suffices, while more severe cases may necessitate surgical intervention.
Sacroiliac Joint Dysfunction
Sacroiliac joint dysfunction refers to misalignment or inflammation of the joints connecting the sacrum to the iliac bones. This condition can be a significant source of lower back pain and discomfort, often radiating to the hips or down the legs. Commonly, it occurs due to degeneration, pregnancy, or repetitive stress injuries, manifesting symptoms that can significantly disrupt daily activities.
Characteristics to recognize include:
- Unilateral pain: Many patients report discomfort on only one side, complicating diagnosis as it can mimic other conditions like herniated disks.
- Pain with specific movements: Activities like climbing stairs or sitting for extended periods may exacerbate discomfort.
Treatment might involve a combination of physical therapy, injections, or in some cases, surgery. It is vital to address sacroiliac dysfunction promptly, considering its potential to lead to chronic pain syndromes if neglected.
Herniated Discs in the Sacral Region
Herniated discs occur when the soft material within a disc protrudes through a tear in its tougher exterior, often compressing nearby nerve roots. While herniations are more common in the lumbar region, they can occur in the sacral area, particularly impacting the sacral nerve roots. Symptoms may vary but commonly include leg pain, weakness, or sensory loss, resembling sciatica-type discomfort.
Some notable points about herniated discs are:
- Distribution of pain: The location of herniation dictates where the pain is felt, with potential symptoms radiating down through the buttocks and into the legs.
- Variation in severity: Some individuals may experience mild discomfort, while others may suffer severe pain and neurological deficits.

Treatments vary based on the severity and may include physical therapy or surgical options for more advanced cases. The goal remains the same: alleviating pain and restoring function. Timely intervention remains essential to avoid complications related to nerve compression.
Diagnostic Approaches to Sacral Spine Disorders
Diagnosing disorders of the sacral spine is a fundamental aspect in understanding its role in both typical and atypical physiological functions. A timely and accurate diagnosis can significantly influence treatment outcomes and ultimately lead to a better quality of life for affected individuals. In this section, we delve into various diagnostic methods that clinicians utilize, offering insights into how these approaches help clarify complex conditions.
Imaging Techniques
Imaging plays a crucial role in diagnosing diseases of the sacral spine. It provides a window into the internal structure, allowing healthcare providers to visualize abnormalities that may not be evident through physical examination alone. The most commonly used imaging techniques include:
- X-rays: While these offer only a basic view, they are vital for assessing structural alignments and identifying fractures. X-rays can swiftly guide clinicians to other more detailed imaging options if necessary.
- Magnetic Resonance Imaging (MRI): This technique is invaluable due to its ability to produce detailed images of soft tissues, such as nerves and discs. MRIs are essential in identifying herniated discs or other degenerative changes in the sacral region.
- Computed Tomography (CT) Scans: CT scans provide cross-sectional images and are particularly useful when evaluating bony abnormalities. These images can reveal fractures that might be undetectable on an X-ray.
Using these techniques, practitioners can pinpoint issues that contribute to pain or instability in the sacral region.
Physical Examination Methods
Physical examinations are the first step in the diagnostic journey. They involve a systematic approach where the clinician assesses the patient’s posture, gait, and physical capabilities. Key methods include:
- Palpation: By applying pressure to specific areas, clinicians can identify tenderness, swelling, or abnormal positioning of the sacral spine.
- Range of Motion Tests: Evaluating the patient’s ability to move in various directions helps determine any limitations or pain associated with specific movements.
- Neurological Assessments: Given the nerves that traverse the sacral region, testing reflexes, sensation, and muscle strength can uncover neurological impacts stemming from sacral spine disorders.
Through these hands-on assessment techniques, a clinician gathers crucial data that could steer the overall diagnostic process.
Differential Diagnosis Strategies
Differential diagnosis is a methodical process that narrows down potential conditions affecting the sacral spine. It's imperative to distinguish between various disorders as treatments can differ vastly depending on the nature of the ailment. Key considerations in this approach include:
- Patient History: A thorough history can reveal patterns or behaviors that might contribute to the condition.
- Symptom Analysis: Understanding the specific characteristics of a patient’s symptoms, including onset, duration, and exacerbating factors, helps in delineating between possible diagnoses.
- Comparison with Similar Conditions: Disorders such as sacroiliac joint dysfunction, lumbar radiculopathy, and fractures can present similar symptoms. Clinicians must leverage imaging and examination findings to differentiate among them successfully.
In summary, the process of diagnosing disorders related to the sacral spine requires a careful blend of technology and clinical acumen. As the medical field advances, new techniques are continually emerging, bringing hope for even sharper and more precise diagnostic capabilities.
Treatment Options for Sacral Spine Conditions
The treatment options for sacral spine conditions are crucial in the overall management of disorders affecting this significant region of the human body. An effective treatment plan not only addresses the immediate symptoms but also considers the long-term wellbeing of the patient. Understanding these options can empower both medical professionals and patients alike, providing insights into potential outcomes and the intricacies of treatment modalities.
A variety of treatment approaches exist, spanning conservative methods to more invasive surgical options. Each approach carries its own set of benefits and considerations, making it vital to tailor solutions to the individual needs of those affected by sacral spine issues. This understanding is particularly relevant given the complexity of the conditions that can arise in this area, impacting mobility and quality of life.
Conservative Management Techniques
Conservative management techniques play a pivotal role in treating sacral spine conditions. Often the first line of defense, these methods focus on alleviating pain and restoring function without the need for surgery.
- Physical Therapy: Structured exercises under professional supervision can help improve muscle strength and flexibility in the sacral area. Targeted stretching and strengthening programs are often effective in relieving discomfort.
- Medication: Over-the-counter pain relief medications, like ibuprofen or acetaminophen, can offer temporary respite from pain. For more intense pain, doctors may prescribe muscle relaxants or stronger pain medications.
- Chiropractic Care: Manual adjustments by a qualified chiropractor can realign the spine and relieve pressure on affected nerves, potentially improving mobility and reducing pain.
- Alternative Therapies: Techniques such as acupuncture or massage therapy have also been noted for their potential in alleviating pain and promoting healing. Though evidence is varied, many patients report significant benefits.
- Lifestyle Modifications: Weight management, ergonomic improvements, and alterations in daily activity can significantly diminish stress on the sacral spine, promoting overall health and preventing further deterioration.
These conservative treatments hold advantage in minimizing risks and often encourage patients to take an active role in their recovery. However, they require time and commitment from patients to achieve noticeable improvement.
Surgical Interventions
When conservative treatments fail to bring relief, surgical interventions may be warranted. Such procedures aim to correct anatomical abnormalities, remove nerve compressions, or stabilize the spinal components.
- Decompression Surgery: This surgery involves removing bone spurs or herniated discs that may be pressing on the spinal nerves. By relieving the pressure, it aims for rapid alleviation of pain and restoration of function.
- Fusion Surgery: In cases where stability is a concern, spinal fusion may be performed. This entails joining two or more vertebrae together, creating a solid bone mass. While this can reduce pain caused by instability, it may also limit mobility in the region.
- Implantable Devices: Some patients may benefit from procedures involving the insertion of devices that help stabilize the spine or relieve pain through electrical stimulation.
Each surgical option presents unique risks and benefits, and the decision to proceed will greatly depend on the specific condition, age, and overall health of the patient. The goal is always to optimize recovery and improve the quality of life.
Rehabilitation Protocols
Rehabilitation following any treatment, whether conservative or surgical, is integral to maintaining improvements and preventing relapses. Rehabilitation protocols focus on restoring the patient’s functional capacity while promoting healing in a structured manner.
- Postoperative Rehabilitation: After surgery, patients often undergo a formal rehabilitation program that may include physical therapy, pain management interventions, and education on body mechanics to minimize future injury risk.
- Continuous Assessment: Regular follow-ups with healthcare providers allow for adjustments in therapy based on the patient’s progress.
- Strength and Conditioning Programs: Tailored strength building routines can help patients regain confidence and physical capability, reducing the risk of further issues.
Overall, effective treatment options for sacral spine conditions hinge on a detailed assessment and a multi-faceted approach. An understanding of each method's implications not just enhances clinical practice but ensures a path towards improved patient outcomes.
Research Trends in Sacral Spine Studies
The exploration of the sacral spine remains an evolving field, continually shedding light on the intricate mechanisms that influence both health and well-being. The relevance of current research trends in this area cannot be overstated, as understanding these developments provide significant insights into the prevention and management of various conditions that can arise in the sacral region.
Emerging Treatments and Technologies
With the continuous advancements in medical technology, treatments for sacral spine disorders have seen a paradigm shift. Emerging approaches combine several techniques to enhance recovery and management of pain. A noteworthy trend is the utilization of minimally invasive surgical procedures, which allow surgeons to address issues with less trauma to the surrounding tissues. Procedures like endoscopic discectomy have led to shorter recovery times, fostering a quicker return to normal activities for patients.
Benefits of these emerging technologies include:
- Reduced recovery time
- Lower risk of complications
- Enhanced precision in surgery
Additionally, some research emphasizes the role of regenerative medicine, such as stem cell therapy. This fascinating field aims to help regenerate damaged tissues within the sacral spine, potentially reducing the need for invasive surgical interventions altogether. Clinical trials are now beginning to show promising results regarding the safety and efficacy of these treatments, propelling this research area forward with the hope of improving patient outcomes.
Genetic and Environmental Factors
Another emerging focus within sacral spine studies is the investigation of genetic predispositions and environmental influences on spinal health. Researchers are examining the interplay between one's genetics and lifestyle choices that may contribute to conditions affecting the sacrum. A comprehensive grasp of these elements can lead to better preventive measures and tailored treatment protocols.

Several factors that are currently under scrutiny include:
- Family history of spinal disorders
- Occupational hazards
- Nutritional habits
Understanding these influences can help target more effective interventions, allowing healthcare professionals to not only treat conditions but also prevent them from manifesting in the first place.
Insights from Recent Studies
Recent studies have provided invaluable contributions to the existing body of knowledge surrounding the sacral spine. Researchers have focused on various aspects, such as improved diagnostic criteria and treatment efficacy. These studies often highlight the importance of an interdisciplinary approach, involving not only orthopedic surgeons but also physiotherapists and pain management specialists when assessing and treating sacral spine conditions.
Insights gained from these studies suggest:
- Early intervention leads to improved long-term outcomes.
- Comprehensive treatment plans addressing both physical and psychological needs can enhance recovery.
- Improved diagnostic imaging techniques, such as MRIs, are crucial in accurately assessing sacral spine conditions.
"Knowledge is power; however, when shared and advanced within the medical community, it becomes a beacon of hope for those suffering from pain and dysfunction related to the sacral spine."
"Knowledge is power; however, when shared and advanced within the medical community, it becomes a beacon of hope for those suffering from pain and dysfunction related to the sacral spine."
Impact of Lifestyle on Sacral Spine Health
The connection between lifestyle choices and the health of the sacral spine cannot be overemphasized. The sacral spine, integral to overall spinal health, is often put to the test by daily activities and habits. From how we move to what we eat, various factors greatly influence the sacral region’s stability and function. Understanding these elements is crucial for preventing injuries and optimizing health outcomes related to sacral spine issues.
Exercise and Physical Activity
Regular physical activity plays a pivotal role in maintaining the health of the sacral spine. Engaging in exercises specifically designed to strengthen the core can provide significant support to the pelvis and lower back. This stabilizing action can prevent discomfort and enhance mobility. For instance, Pilates and yoga have garnered attention for their emphasis on core engagement and flexibility.
- Benefits of Exercise:
- Increased blood circulation to spinal structures.
- Improved muscle tone and strength.
- Enhanced flexibility in the pelvic area.
Moreover, low-impact activities such as swimming or cycling can augment endurance without placing excessive strain on the sacral region. The key is consistency; a sedentary lifestyle may lead to weak muscles, making the lower back more susceptible to injuries.
Ergonomics and Posture
The significance of ergonomics in daily tasks from working at a desk to lifting objects is often underestimated. Maintaining proper posture can greatly reduce undue pressure on the sacral spine. Common issues arise when individuals slouch while sitting or overextend while standing.
To incorporate good ergonomics:
- Adjust your seating: Use chairs with good lumbar support.
- Monitor heights: Your computer should be at eye level to minimize neck strain.
- Practice awareness: Regularly check in with your body position throughout the day.
These steps can prevent muscle fatigue and strain, helping maintain the natural curvature of the spine. Even minor adjustments in posture can lead to significant improvements in sacral health over time.
Nutritional Considerations
Nutrition equally plays a fundamental role in sustaining a healthy sacral spine. A well-balanced diet rich in anti-inflammatory foods can combat the degenerative changes affecting spinal structures. Prioritizing nutrients such as calcium and vitamin D can fortify bone health, reducing fracture risks in the sacral area.
Some effective dietary choices include:
- Leafy greens for calcium.
- Fatty fish like salmon for omega-3 fatty acids.
- Nuts and seeds for healthy fats and protein.
In addition, staying hydrated is essential as it maintains the elasticity of spinal discs. Neglecting hydration can lead to disc degeneration, exacerbating back pain and affecting overall mobility.
"An ounce of prevention is worth a pound of cure." - Benjamin Franklin
"An ounce of prevention is worth a pound of cure." - Benjamin Franklin
By adopting a comprehensive focus on exercise, ergonomics, and nutritional habits, individuals can significantly enhance the health of their sacral spine. These practices not only improve stability and function but also contribute to a better quality of life in general.
Ending
Concluding this exploration of the sacral spine immerses us in the richness of its anatomy and function while recognizing its pivotal role in health and well-being. The sacral region is not just a mere collection of bones; it stands as a key player in both structural integrity and neurological pathways.
In summary, understanding the sacral spine offers several advantages:
- Awareness of Conditions: Recognizing the common disorders associated with the sacral spine—such as sacral fractures and sacroiliac joint dysfunction—enables proactive healthcare management.
- Enhanced Treatment Protocols: A nuanced grasp of the sacral anatomy informs clinical practices, allowing for tailored treatment options that cater to individual patient needs, potentially leading to better outcomes.
- Integration of Research: Engaging with the ongoing research trends related to the sacral spine uncovers emerging treatments and technologies permitting advances that benefit both clinical practice and academic inquiry.
Taking all this into account, it’s evident that the conclusion of our discussion is not just an endpoint but rather a junction that connects past insights with future explorations. Medical professionals, educators, and researchers alike can benefit from this broad spectrum of knowledge, fostering a deeper appreciation for how elements of sacral function impact overall health.
**"Knowledge is power, and understanding the role of the sacral spine enhances our ability to provide comprehensive care."
**"Knowledge is power, and understanding the role of the sacral spine enhances our ability to provide comprehensive care."
Summary of Key Insights
Throughout the discourse, various critical points emerge that encapsulate the significance of the sacral spine:
- Anatomical Complexity: The sacrum, through its unique structure, supports both posture and pelvic stability.
- Functional Relevance: It plays a vital role in load transfer, contributing to the overall biomechanics of human movement.
- Clinical Considerations: Awareness of sacral conditions aids in proper diagnoses and informs treatment strategies, ultimately enhancing patient care.
Leaning on these insights not only elevates the understanding of healthcare providers but also encourages patients to be more engaged in their own health journeys.
Future Directions in Sacral Spine Research
Looking ahead, it’s crucial to recognize how the field continues to evolve:
- Technological Advancements: Innovations in medical imaging and surgical techniques promise to improve diagnostic accuracy and treatment efficacy.
- Interdisciplinary Approaches: Collaborations among neurologists, orthopedic specialists, and physiotherapists could open new avenues for comprehensive sacral spine management.
- Longitudinal Studies: Ongoing research into the long-term effects of lifestyle factors on sacral spine health could illuminate preventative measures and health strategies.



